
(UPDATED May 1, 2023)
As the weather warms up and summer approaches, many of us are getting excited for weekend family hikes, outdoor BBQs and camping trips. I know I am!
But unfortunately, with the great outdoors, comes the not-so-glamorous reality that there are lots of creepy crawlies out there that can transmit some pretty nasty infections. Yes – I’m talking about TICKS! EEUUWWWW!!! There’s nothing quite as prehistoric-looking and spine-tingling as a tick (except for maybe a cockroach). And the knowledge that the blacklegged deer tick (Ixodes scapularis) – tiny creatures as small as a poppy seed or a sesame seed – can transmit infections such as Lyme disease (Borrelia), Bartonella, Babesia, Erhlichia, Anaplasma, Tularemia, Rocky Mountain spotted fever, relapsing fever, Colorado tick fever, Powassan virus, just to name a few, make them seem somehow even more like something out of a sci-fi horror movie.

The blacklegged deer tick
And if you think that Lyme disease from blacklegged deer ticks is just a concern on the East Coast – think again. A Stanford study in 2014 found that nearly every park in the San Mateo, Santa Clara, Santa Cruz and Mendocino counties that was sampled (these are the parks that I hike with my children!) had ticks that were infected with Borrelia spirochetes (the organism responsible for Lyme disease). Another Stanford study in 2015 sampled additional parks from Sonoma County to Santa Cruz County and confirmed that virtually all of the parks contained ticks that were infected with Borrelia spirochetes, including a newly identified species called Borrelia miyamotoi.
And shockingly, a report in 2019 by the CDC shows that tickborne and mosquito-borne infections have TRIPLED over the last 13 years. (1) This includes Lyme disease, which accounts for 82% of all tick-borne diseases. And the authors note that “underreporting might have substantially limited the number of cases analyzed. As noted, the number of Lyme disease cases reported to NNDSS is estimated to represent a fraction of incident cases.” So the number is likely actually MUCH HIGHER!
(If you want to cut to the chase and know what to do if your child gets bitten by a tick, DOWNLOAD my FREE GUIDE HERE!)
Why Worry About a Tick Bite?

The biggest concern with getting a tick bite is the risk of transmission of a tickborne illness. Lyme disease takes the spotlight, with horror stories abounding on the internet, but Babesia and Bartonella can be just as devastating. In children, these infections can become an autoimmune encephalitis called PANS (Pediatric Acute-Onset Neuropsychiatric Syndrome), of which PANDAS (Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal Infections) is a subset. Children with PANS/PANDAS develop a sudden-onset of fears, anxiety, OCD behaviors, rages, tics, bedwetting, handwriting regression and brain fog after exposure to certain infections or toxins. An infection like Lyme or strep can trigger an autoimmune, inflammatory reaction in the brain that results in neuropsychiatric symptoms – their brains are literally on fire. PANS/PANDAS and chronic pediatric Lyme disease have become a very large part of my holistic pediatric practice, and while I have been able to thankfully help many of these children recover from this devastating illness using a holistic integrative approach, my preference would be that kids never got it in the first place! And one of the first steps is making sure that we as parents know exactly what to do when our children get bitten by a tick.
(Side note: PANS/PANDAS is such an important issue that I have been interviewed about it to educate other functional medicine practitioners. You can listen to my 2-part interview on Fx Medicine Australia HERE: PANDAS Part 1 and PANDAS Part 2 and my interview with Dr. Kara Fitzgerald on New Frontiers in Functional Medicine HERE: Functional Medicine Pediatrician Dr. Song on PANS/PANDAS Dx and Treatment)
Prevention is Key
The first and most important step is to try to PREVENT a tick bite in the first place. Prevention includes the following key steps:
- Stick to the middle of well-cleared paths. Ticks like to live in tall grassy areas and jump onto your skin as you’re walking by brushing up against the grass, or sitting on a log under a tree to cool down. Make sure that the kids don’t wander into tall grassy or shrubby areas. This is definitely not the time to be going off trail!
- Wear the right clothing, in the right way! Ticks can crawl under your shorts or down your shirt to find a nice warm place to take a bite and burrow in. As “uncool” as it may look, be sure to wear long pants and long sleeves and keep your pants tucked into your socks, and your shirt tucked into your pants so there are fewer potential points of entry. Lighter-colored clothing and socks make it easier to spot a tick on your clothes before it finds a way inside, so you can brush it away before it can even take a bite.
- Frequently apply a safe and effective insect repellent that works against ticks. I’m not talking about DEET, which I don’t recommend for routine use because of its associated toxicity. You may want to consider permethrin-treated clothing if your child will be spending an extended period of time outdoors in nature (I don’t use this for my kids, and I don’t recommend it for use on the skin directly as there is still toxicity associated with permethrin, especially with excessive use). Several studies have found various essential oils to be effective in repelling and killing ticks. A 2004 study found a lemon eucalyptus extract to be effective in reducing the risk of tick bites. A 2008 study found tansy essential oils to be very effective in repelling ticks by up to 64-72%. Other essential oils that may be effective tick repellents include rose geranium (aka Pelargonium graveolans), clove, lavender, palmarosa, pennyroyal, rose, and sweet myrrh.
If you’re a DIY kinda person, you can certainly make your own essential oil-based sprays, lotions or wipes. Or, if you’re like me and prefer something ready-made, you can try one of the following:
- Nature’s Cloak Mosquito, Tick and Insect Repellent with lemon eucalyptus, lavender, rose geranium, lemon tea tree and cedarwood essential oils
- Badger Bug Repellants with citronella, cedar, lemongrass, rosemary, geranium, and peppermint essential oils
- Fedorenko’s Bug Stick with lemongrass, citronella, peppermint, rosemary, cedar, clove, and geranium essential oils
Regardless of which essential oil product you choose to use, the key is to apply frequently, every 2-3 hours or more frequently after sweating or swimming. Remember – essential oils are effective because of their scent. If you can’t smell it, chances are a tick can’t smell it either and won’t be repelled appropriately.
- Do frequent tick checks. Ideally, you’ll find a tick crawling on your child’s clothes before it ever has a chance to bite, and just be able to flick it away. But if a tick has bitten, the earlier you find it, the less time it’s had to transmit its saliva that carries the Borrelia spirochetes and other bugs, and the less likely you are to contract Lyme disease and other tickborne infections. Just because a tick carries Borrelia and bites you does NOT mean that you will get Lyme disease. While it’s not entirely clear “how long” a tick needs to be embedded in order to transmit infection, it’s clear that the longer a tick is attached, the higher the risk of transmission. It has previously been thought that the tick must be attached for more than 24 hours to transmit Lyme, but it now seems that just a few hours may be enough – although the risk is much greater if the tick has been attached for over 24 hours. So early tick detection and removal is key to preventing Lyme disease.
While you’re out on the trails, take time to periodically scan their body for ticks. Carefully check behind and in your child’s ears, back of the neck, hairline and run your fingers through your child’s scalp. Look under the collar of their shirt and in their armpits. Check their waistline under their pants and any other possible points of entry. You are literally going to be looking for something that looks like a speck of dirt or a new freckle that you hadn’t noticed before. The nymph, the smallest form of the deer tick that is most prevalent in spring/summer, is literally the size of a poppy seed. Until you actually find one embedded, it can be difficult to appreciate just how tiny and difficult to spot they are!
Once you’re back home, take your child’s clothes off and wash in hot water or put in the dryer on high for 30-60 minutes. Take a warm shower IMMEDIATELY to wash away ticks that haven’t fully attached yet, and do another thorough tick check after the bath. Be as thorough as possible because most people with Lyme disease never notice the tick that gave it to them. Ticks love warm, moist, dark areas of the body so check hidden areas especially in or around the ear, hairline and scalp, bellybutton, armpits, groin/genitalia, or areas where clothing was pressed against the skin (waistline, underwear line, neckline).
- Check your pets. Pets can carry ticks into your home after being outside. They can also contract Lyme disease, so be sure to do a thorough tick check after you’ve taken your dog for a hike, or if they’ve just romped around your backyard that deer and other animals sometimes frequent.
- Check your gear. If possible, wash your backpacks and camping gear, or at the very least do as thorough an inspection as you can and shake everything out. A little tick found its way home from one of our camping trips, and being so tired, I just put away Kenzi’s unworn clothes back into her drawers instead of washing first (I know! What was I thinking?!?!). Of course, the next morning, Kenzi goes to put on some socks before we head out to school, and comes back and asks me what the little bump on her leg is! I knew it had only been attached for possibly 5 minutes, so I didn’t panic (much), and followed the plan outlined below.
What to do if your child gets a tick bite

The first thing to do when you find a tick on your child:
STAY CALM and DON’T PANIC!
The first time I found a tick on my son after we had been swimming in a river in Mendocino County, I thought there was a speck of dirt on his chest. But when I tried to flick it off and it didn’t budge, my heart sank and my stomach churned because I knew exactly what it was. It took everything in me to not freak out and show the panic in my eyes as I was gently pulling it out, all the while holding my breath. The next time I found a sesame seed-size tick was in my daughter’s ear while I was giving her a bath after she had been playing in our front yard. (We live in a suburban town in the Bay Area, but we do have deer that sometimes wander through our yard from the hills, so I’m sure some deer ticks were deposited on our grass as they were passing by – yikes!). Even this second time around, I thought it was a speck of dirt and tried to pick it off with my finger nail. I didn’t feel any less like freaking out, but somehow I managed to keep it together!
The second thing is to REMOVE THE TICK.
How to remove a tick
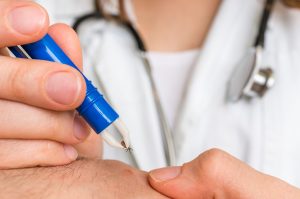
There are several things you should NOT do when your child has a tick bite, besides not panic.
DO NOT use Vaseline, gasoline, fingernail polish, rubbing alcohol, or any other caustic substance on the tick.
DO NOT put a lit match next to the tick or squeeze or crush it.
Doing any of these can inadvertently cause the tick to regurgitate more of its saliva that carries Borrelia and other infections into your body.
What you SHOULD do:
- Have a small Ziploc bag open and ready.
- Use fine-tipped tweezers to grasp the tick as close to the skin as possible without crushing it. Pull with gentle steady pressure up away from the skin. BE PATIENT. Keep the pressure steady. This is where you might find yourself holding your breath trying not to scream like I did. Don’t twist or jerk up as this may cause the tick to break off leaving its mouthparts still embedded in the skin.
- After a little while, you’ll feel a sudden give as the tick releases its hold. DON’T PANIC and drop your tweezers! Gently put the tick into your Ziploc bag and close it (or if you’re like me, drop the tick, tweezers and all and zip that bag as fast as you can and then breathe because you’ve just been holding your breath for 5 minutes). Place a small moist cotton ball or piece of paper towel in the Ziploc bag so the tick doesn’t dry out before you send it for testing.
- If you’ve pulled out the tick but the head and mouthparts are still embedded, don’t dig around and try to get it out. Head to your local urgent care or your doctor to safely remove it completely.
- Immediately wash the area with warm water and soap, and apply tea tree oil or any other antiseptic that you have on hand.
- Note the site of the tick bite, and draw a circle with a ballpoint pen around the bite site so that you remember where it is.
(There are various tick-removing devices available. I’ve tried a few but I honestly haven’t found any as effective as a pair of good ‘ol-fashioned tweezers)
What To Do After a Tick Bite
Now that the tick is successfully removed, what next? What do you do with that little baggie holding that fear-inducing poppy-sized vermin? Do you give you child antibiotics? Do you just wait and see if your child develops symptoms of Lyme disease?
Remember: The goal is to PREVENT LYME DISEASE. Lyme disease, if caught early and treated appropriately does NOT have to go on to be a devastating chronic illness.
Get the Tick Tested
The first thing I recommend doing immediately once you’re back home is to send the tick to a lab to determine whether or not it even carries Lyme or other tickborne infections. Some labs (including most public health labs) will only identify whether the tick is a blacklegged deer tick, and only if it is, will they test to see if it carries Borrelia burgdorferi. While knowing what kind of tick it is may be useful, it is more important to know whether the tick actually carries any infections. I do recommend checking for co-infections, and not just for Borrelia alone. Ticks can carry and transmit more than one infection, and knowing what symptoms to watch for can be very helpful in early diagnosis. One of my daughter’s ticks tested positive for Ehrlichia which she fortunately did not develop, and I was thankful to know to look for any subsequent symptoms of Ehrlichiosis rather than Lyme disease.
I recommend tick testing through a lab like TickReport, TickCheck, or Ticknology. The turnaround time for these labs is 3-5 days from receipt of the tick. But in the meantime, while you’re waiting for results, you’re still stuck with the question of whether or not to take prophylactic antibiotics.
Should I Give My Child Antibiotics?
To take prophylactic antibiotics or not – that is the question. Prophylactic antibiotics may prevent the development of Lyme disease if given as soon after the tick bite as possible. One study showed that a single 200mg dose of doxycycline given within 72 hours of tick attachment may be effective in preventing the classic erythema migrans rash within 4 weeks of a tick bite; however, the development of a rash is not necessarily a good endpoint as many people with Lyme disease never develop a rash, and this study had no long-term followup to determine if patients went on to develop symptoms of chronic Lyme disease. Most Lyme-literate practitioners do not believe that a single dose of antibiotics is adequate to prevent Lyme disease, and that at least a 3-week course of antibiotics is needed to ensure that you kill the Borrelia in all of its life forms – the free-floating spirochete form, the evasive cell wall-deficient form, and the dormant cyst form. If you stop antibiotics too early, you may not kill the Borrelia that is hiding out in its dormant cyst form and waiting for just the right moment to reactivate and convert to its free-floating spirochete form to cause trouble at a future date.
But antibiotics? Are they really necessary? And especially if your child already has gut issues, or you’ve worked so hard to heal their gut? While a tick is unlikely to transmit Lyme and coinfections if it has been attached for less than 24 hours, there have been reports of transmission after just 16 hours. So, if you think that a tick has been attached for more than 16 hours, and especially if it looks engorged with blood, then in this case, I would strongly consider antimicrobial support. After caring for too many children and parents with chronic Lyme disease and other tickborne infections, I would rather mop up the after effects of gut dysbiosis and increased intestinal permeability (“leaky gut”) than mop up the after effects of chronic Lyme disease.
How long should you/your child take antimicrobials? At least while you’re waiting for the tick test results to come back. If the results are negative for any tickborne infection, then you can stop the antimicrobial. If you did not send the tick to be tested, or the tick test comes back positive, the antimicrobial(s) chosen should be taken for a minimum of 3-4 weeks.
Which antimicrobial should you/your child take? The antimicrobial chosen may be herbal or pharmaceutical, or a combination of both. For adults, a 3-week course of Doxycycline may be recommended. Theoretical concerns regarding teeth staining with Doxycycline in children under 8 years of age no longer seem to be warranted, and the CDC now recommends “doxycycline as the treatment of choice for children all ages with suspected tickborne rickettsial disease… Previous concerns about tooth staining in children aged <8 years stem from older tetracycline-class drugs that bind more readily to calcium than newer members of the drug class, such as doxycycline.” In fact the 2018 AAP Red Book states that “doxycyclne can be used for short durations (i.e., 21 dys or less) without regard to patient age …” Amoxicillin and Azithromycin are alternative antibiotic choices for children. Herbal antimicrobials targeted to Lyme and coinfections can also be used alone or in combination with pharmaceutical antibiotics. Just remember, though, that herbal antimicrobials can still disrupt the gut microbiome like antibiotic drugs, and the gut needs to supported just as fully as outlined below. The manufacturers that I recommend for herbal formulas for Lyme and coinfections include BioResource, Researched Nutritionals and Beyond Balance.
Stephen Buhner, a highly regarded Lyme herbalist, recommends the herb Astragalus with adult dosage of 3000mg daily for 30 days after a new tick bite. For prevention, Buhner recommends that adults take Astragalus 1000mg daily during your time in a Lyme-endemic or tick-infested area may be helpful in boosting your immune system and preventing Lyme transmission. This may be a good option for you and your family if you live in a high-Lyme area and don’t want to potentially be on antibiotics for the entire season… Immediately after a tick bite, Buhner has also found applying a topical paste made of andrographis tincture and green clay to be helpful in preventing infection.
If you or your child does get bitten by a tick, please discuss what antimicrobial regimen is best with your physician or a Lyme-literate practitioner.
Bottom line: I would strongly consider giving your child an antimicrobial medication, pharmaceutical and/or herbal, for at least 3-4 weeks after a tick bite, especially if you believe the tick was attached for more than 16 hours and looks engorged.
How do your support your child’s gut with antibiotics?

Kimchi – Korean pickled cabbage
The gut can and should be fully supported while taking antimicrobials for Lyme prevention – whether they’re pharmaceutical or herbal. The goal is to minimize disruption to the gut microbiome and prevent gut dysbiosis and leaky gut (and yes, even herbal antimicrobials can cause gut dysbiosis). Be sure to give your child probiotics at least 1-2 hours after each antimicrobial dose, and continue for a month after the antimicrobial course is complete. To help you choose the best probiotic for your child, you can download my Guide to Choosing Your Child’s Probiotic. Load up on fiber-filled plant foods and awesome fermented foods like sauerkraut, beet kvass, “real” pickles like Bubbies, kimchi, miso soup, kombucha, coconut kefir and yogurt (if you tolerate dairy). Drink bone broth for all that healing glutamine and gelatin to support the small intestinal lining and prevent leaky gut. And be sure to eat a whole foods diet full of variety and color to ensure that your child’s gut gets all the phytonutrients it needs to stay healthy during this time.
Watch for Signs of Lyme Disease
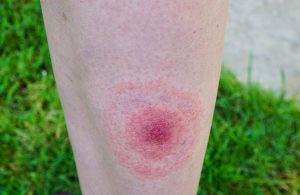
Erythema migrans – the “classic” bullseye rash of Lyme disease
While the above precautions can be very effective in preventing Lyme disease, there may still be occasions where it’s not enough. Watch the site of the tick bite for an expanding bullseye rash, and watch your child for symptoms of acute Lyme disease. Only about 50-60% of patients with Lyme disease ever develop the classic “bullseye rash,” or erythema migrans, with a red ring that expands outward from the site of the bite. The vast majority of people with chronic Lyme disease never recall having a rash, so you want to watch for the other signs and symptoms of Lyme disease to know when to go see your doctor.
Acute Lyme disease can develop anywhere from 3 to 30 days after a tick bite so you’ll want to be on guard for at least a month. Although again, if you’ve taken the above precautions, the chance that your child will develop Lyme disease is significantly lowered and you can breathe a little easier!

Go immediately to your physician if you or your child develops any symptoms of early or late Lyme disease below. The following list can also be found in a convenient Lyme Symptoms Handout from the Bay Area Lyme Foundation. Remember, most people with Lyme disease don’t remember being bitten by a tick, so for some, late-stage Lyme symptoms will be their first sign of Lyme disease.
Early Localized Stage (days to weeks after tick bite)
- Skin rash, commonly — but not always — a circular or bullseye rash around the bite area
- Headaches or stiff neck
- Flu-like ailments, including fever or chills
- Muscle and joint pain
- Profound fatigue or lack of energy
- A small bump or redness at tick bite
- Swollen lymph nodes
Early Disseminated Stage (weeks to months after tick bite)
- Expanding skin rash (more or larger rashes covering more parts of the body)
- Pain or numbness in arms and legs
- Extreme joint pain
- Profound fatigue
- Headaches and lack of energy
- Fainting
- Bell’s palsy (facial paralysis)
- Poor memory or inability to concentrate
- Heart palpitations
Late-Stage Lyme (months to years after tick bite)
- Arthritis, particularly in the knee or near the point of infection
- Nervous system problems including numbness and tingling in hands, feet, or back
- Severe headaches or migraines
- Problems with memory, hearing, and vision
- Stiff neck due to swollen tissues
- Chronic fatigue
- Problems with mood or sleep
- Inflammation of the brain
- Inflammation of the heart
PLEASE NOTE that in children, symptoms of Lyme may also include behavioral changes (anxiety, depression, fears, OCD behaviors, tantrums/rages), tics, developmental regressions (i.e., deterioration in handwriting), brain fog, slowed cognitive processing, and memory problems.
If your child does develop signs of Lyme disease, please demand that your physician order more specialized Lyme testing through a lab like IGeneX or at the very least order a complete Lyme IgG and IgM Western blot and not simply a Lyme antibody screen with a reflex to Western blot. Unfortunately, the diagnosis of Lyme is highly controversial, but you do NOT want to miss a diagnosis of Lyme disease. Due to the inaccuracy of current testing methods, even the CDC recommends basing the diagnosis of Lyme on clinical symptoms and not on laboratory findings. If your physician will not test appropriately or is not well-versed in Lyme disease, please find a Lyme-literate practitioner near you through ILADS (International Lyme and Associated Diseases Society).
What else can I do to prevent Lyme disease?
I often wonder why it is that some children go on to develop PANS or chronic Lyme disease from a tick bite, and other kids do not? Why do some adults go on to develop chronic Lyme disease with devastating neurologic symptoms, and others develop no symptoms at all?
I believe some of the answers lie in:
- Early detection and treatment
These are all the steps that you’ve already taken above! 😊
- Supporting any suspected underlying methylation or mitochondrial dysfunction
Many of the kids that I see with chronic illness, including PANS/PANDAS, have subtle red flags that they may have had underlying methylation and mitochondrial dysfunction that predisposed them to a greater risk for complications and long-term effects of certain chronic illnesses. These red flags include low energy, poor endurance, sensory issues, regressions after illness or prolonged recovery time compared with peers. They also include a family history of autoimmune illness, atopic disease (eczema, asthma, allergies), neurodegenerative disorders (autism, Alzheimer’s, Parkinson’s, etc.), mental health disorders, infertility, blood clotting disorders, and early heart disease.
If your body is trying to fight off Borrelia or other tickborne infections, its methylation and mitochondrial stress have increased. If your methylation and mitochondrial function is already impaired, then this added stress can tap out your reserves and be the proverbial “straw that broke the camel’s back,” so that what seems like a sudden development of neuropsychiatric symptoms is really the culmination of a long backstory of previous methylation, mitochondrial, immune, and detoxification stressors.
How do you support your child’s methylation and mitochondrial function? After a tick bite, you can add supportive supplements like methyl-B12, l-methylfolate (or L-MTHF), coQ10, ribose, and L-carnitine.
But we’re talking about true prevention. So even before that tick bite ever occurs, optimize your whole family’s health with the steps below to bolster everyone’s defenses.
- Optimizing health
Optimal health begins with the gut and ends with the heart. Optimal health means supporting body, mind, and spirit with the following steps:
- Ensure a healthy gut microbiome with fermented foods, bone broth, and probiotics.
- Eat a diet rich in whole, unprocessed, organic foods with a variety of phytonutrients (a rainbow of fruits and vegetables), healthy fats and wild, free-range proteins.
- Avoid pesticides, heavy metals, and artificial flavors, colors and preservatives.
- Supplement lacking or insufficient nutrients such as omega-3 essential fatty acids (i.e., fish oil), vitamin D3, zinc, and magnesium.
- SLOW it down and teach your kids to manage stress through mindfulness and meditation (for tips on how to do this, see my blog post on the Holistic Management of Anxiety.
- Get outside in nature as often as possible (while watching for ticks!).
- Get enough sleep! Check out my blog posts on sleep: The 3 Things You Need to Know to Get a Good Night’s Sleep and Eat Yourself to a Good Night’s Sleep.
There you have it! All the steps you need to take if you or your child gets a tick bite!
Knowledge is Power!
Armed with the right information, your whole family will enjoy a healthy, happy summer in the great outdoors!
Be sure to download my FREE GUIDE on What To Do If Your Child Gets a Tick Bite to have on hand whenever you need, and be sure to share with any friends or family who want to know how to enjoy the great outdoors without worry!

Thank you so much for taking the time to read this very important blog post on how to prevent and treat tick bites and hopefully prevent chronic Lyme disease. Please share with any family who loves spending time outdoors in nature, so we can all do our best to keep our children healthy and happy for a lifetime!
xo Elisa Song, MD
Thank you for this article. My son had a tick at the back of the neck. He was away with his father and complained of a sore neck Friday evening Howe we it was Sunday lunch before I saw him and discovered the tick. We removed it and had it tested, and it was Lyme carriage. We had gone straight to urgent care and started antibiotics immediately for the course of 2 weeks I think. After the tick results came in we blood tested my child and he had no antibodies of exposure. Should I still be worried? It’s been almost two years
Hi Shae,
Remember, not everyone who gets a tick bite will get Lyme, even if the tick has been attached for a long time. If your son is healthy and developing normally and thriving, then I wouldn’t worry and just do your best to keep him as healthy as possible!
xo Elisa
Thank you, Elisa, for this really balanced and comprehensive article. Here in the French Alps tick-borne diseases are endemic but there is surprisingly little awareness of them, let alone prevention. As a result, even in our village, I know of several people trying to cope with chronic Lyme, which is not always recognized as such by the medical establishment. A few years ago I developed an erythema migrans rash but immediately knew what it was and got 4 weeks of antibiotics resulting in no further symptoms. Your focus on knowledge and prevention is certainly the key. I don’t have young children at home now but always find your articles interesting and informative.
Hi Mary – Thanks so much for your kinds words! Yes – knowledge is power so hopefully more and more people become Lyme-aware…
xo Elisa
OMG! Get the tick repellant that is not toxic and works! From Montana Farmacy also on Etsy, or make it yourself with essential oils. The recipe is in the book “HEALING LYME”.
If you get bitten, use andrographis tincture and bentonite clay on the bite. Be prepared, have it on hand. Take 1-2 grams Astragalus everyday to prevent Lyme and other infections. Throw it in juice or a smoothie, or take it by the spoon or capsule.
Thank you for your thoughtful comment!
🙂 Elisa
Thanks for this. Another acupuncturist momma told me she gives her kids ledum homeopathy after they get tickS. Would you do this too? If so, what dose and for how long?We check ourselves throughout the day and every night. I’ve already found 5 ticks bites in my 21mo son this year. (One was in his scalp which I found by chance… I don’t even know how to check the scalp so I just look through it whenever I get a chance.) anyway, if I followed the antibiotic recommendation then he would have been on them for several months already. Luckily we do many healthy practices and I think he is ok. Ooh- such a rich topic… I could go on….
Hi Rachel,
Ledum may be helpful in preventing insect and tick bites, but I don’t know that it would prevent Lyme transmission after a tick bite. However, to use it preventatively, many people will take Ledum 9C or 30C 3 pellets 2x/day when going in a mosquito or tick area. I do like Steve Buhner’s recommendation for astragalus when in a Lyme-endemic area for a prolonged time, because yes – for many kids they would potentially be on antibiotics year-round! Best of luck! There are no clear dosage guideliness of astragalus for kids. But it generally is considered safe, although I would use caution if you have an autoimmune illness. Best of luck!
Elisa
Thanks! Found another one on him again today, ugh. What form is easiest to give astragalus to kids? is there a glycerin tincture? could i put it in his morning oats?
thanks again.
Hi Rachel! Herb Lore (www.herblore.com) makes a great glycerin-based astragalus tincture. Herbs for Kids makes one as well. I’ll put a post soon on different strategies to get supplements into kids :-), but yes – in oatmeal, a little bit of smoothie, or apple sauce are all options!
xo Elisa
Do you do treatment for kids with Pandas? Both mine have been diagnosed and have been on ABX almost a year with only small improvements in their streph titres.
Hi D’Anne. Yes, my partner Dr. Trolan and I both treat kids with PANDAS. I’m so sorry for your struggles! PANDAS can be so devastating. I wish you and your children the best. If you would like to consult with our practice, Dr. Trolan practices in the very same was as I do and is currently accepting patients. You can go to http://www.wholefamilywellness.org for our practice information. Best of luck!
xo Elisa
Thank you Elisa, such a great and informative post. Just a question though, you are most likely to be outdoors when you have a tick bite – so any tick removing advice for when you are outdoors? (When you won’t have access to tweezers or zip doc bag)?
Hi Vivian! You know, when I’m going to be hiking or outdoors, now I actually always carry a baggie and tweezers with me… Otherwise, if you don’t have access to supplies and won’t be back home within an hour or two, I would pull the tick out as carefully as possible with your fingers if you can and then watch closely for symptoms of Lyme or coinfections. Take care!
Elisa
Great article! Thanks so much for this thorough article. You can get the tick tested through UMASS. I had my complete results from my test within six days of mailing my tick. I live in San Francisco and sent the tick with Priority Mail. The cost for a complete test (with additional tick-born diseases besides lyme) and turn around are much better than any other company I researched.
Thx, Daniela! Leaving off Tick Report was my oversight. Thx for reminding me! I added them in as a resource, as well as a reminder to check for co-infections.
🙂 Elisa
Hi, My family and I were camping over Memorial Day near Manteca CA(Friday to Monday). The Mosquitoes were fierce so we kept well covered and used bug spray… no showers for 4 days. On Tuesday AM I saw a bit on my almost 9-year-old’s shoulder that looked different from the rest. It was very symmetrical and about the size of a quarter. It wasn’t raised much or puffy like the rest. My son said it didn’t itch like the rest. I watched it fade for a week with little alarm (but took picture along the way). Yesterday my son woke up with a larger, darker bullseye beyond the original boundary. We went to his pediatrician that day. The pediatrician insisted we would have seen the tick. No tick, no Lyme he said. He’s certain it is just a secondary infection from scratching. I did mention that all his bites were scratched to the point of bleeding and wondered if he could have scratched the tick out himself. He said no way. He does still have other inflamed bites that are quarter sized but they are raised, not symmetrical, and still itch. This one doesn’t itch and hasn’t been itching. He thinks the bite behaves different from the rest because it was a spider and the rest were mosquitoes.
He explained that Doxycycline would not be given to my son because of he age. I asked about Amoxicillin and Azithromycin. He said studies say they don’t work. The doctor is sending pictures to the infectious disease department of Kaiser. My son was given a 10 day course of Cehphalexin to fight the bacterial infection and topical Hydrochrtisone. He told me to watch for flu symptoms.
Should I follow his directions or get a second opinion? I found you because you are the pediatrician to my friend’s family and she suffers from Lyme’s Disease herself.
Oh my goodness, Laura – what a quandary. Most infectious disease doctors would say if there is a bullseye, that is “pathognomonic” for Lyme disease (meaning not really anything else does that), and would go ahead and treat. The difficulty is that there is conflict between ILADS (Lyme-literate docs) and IDSA (conventional ID docs) about how to diagnose and treat Lyme disease. If it really does look like a bullseye, however, I would take my child in for a second opinion. The Bay Area Lyme Foundation has great resources, including this link to an article on their page http://www.bayarealyme.org/lyme-disease-prevention/protect-yourself-your-family/ which points out that most people DON’T notice a tick bite. Click on the link on their page that reads: “See this article from the California Lyme Disease Association and Sonoma Mosquito & Vector Control”.
Best of luck!!!
Elisa
Thank you for your comprehensive article and for responding to my reply so quickly. Please thank your staff for me as well. I called them today, and they were very helpful in giving me the names of Lyme specialist in the area. I have a second opinion scheduled for early next week with a Lyme specialist. Who knows where this will go. It just feels good to know I’m doing all I can to help my son stay healthy. Really, thank you!
You’re so welcome! Best of luck!
Definitely seek out a Lyme literate doctor. My daughter had a homogeneously red circular rash (not bull’s eye and not expanding and also did not itch). I went to multiple doctors within Kaiser, and they all refused to treat with antibiotics, thinking that it was not Lyme. Along with their ignorance of diagnosing Lyme, they also were not knowledgeable at treating Lyme and its co-infections. I contacted ILADS and took her to a Lyme literate doctor. It turned out that she had 3 co-infections, along with Lyme. Infectious disease doctors do not treat long enough to typically treat the infection. Also, multiple medications may be needed to treat various co-infections. My daughter is on three antibiotics, one anti-malarial med. and one herbal (along with good pro-biotics) and has been for many months. After 9 months of treatment, she has just recently lost most of her symptoms. They were subtle and difficult for us to detect. Please seek out a Lyme specialist to make sure you treat your son accordingly now. Godd luck!
Yes yes yes, Penny! So important to work with a Lyme-literate doctor who is familiar with the ILADS approach… Thank you!
xo Elisa
My mother will take our almost 12 yr old son for a 10 day sailing trip around Santa Cruz Island off the coast of Southern CA in July. They anchor, hike, Snorkel, etc…. although there are trails-they often do get overgrown as less and less people do this anymore… and with the rain I am a little concerned about ticks.
I have Hashimotos and my husband has MTHFR gene mutation -so we are familiar with autoimmunity and hope to help our son prevent this…. but while my mom will give token concern to ticks- I don’t think she is vigilant at all….
so my concern is that I won’t be able to check my son til after about 12 days from his first exposure.
If my mom actually finds a tick…. but we can’t get medicine for 12 days… how bad is this?
I am wondering if I should try to get a Dr to give us a dose of Antibiotics-for them to take with them just in case?
The island is 25 miles of the coast- it is a 6 hr sail on average -with only Coast guard radio -ship to shore communications… no cell service.
Any feedback you might have would be great!
Hi Shannon,
What an amazing adventure for your son! But yes, ticks could be a concern. Your son can definitely be involved in doing his own tick checks so you can practice that even while you hike before he leaves. It may be challenging to find a doc who is willing to write a prescription for prophylactic antibiotics… I know for my daughter who will be at outdoor Girl Scout camp for 2 weeks, I am planning to give her astragalus 500mg daily… I also will have a ziploc bag and tweezers in her backpack at all times.
Best of luck!
Elisa
This is a fantastic article. Thank you!
You mention deer as the primary culprit for transporting ticks, but my understanding is that they hitchhike on mice and chipmunks more frequently, which is why ticks and ticknorne illnesses are an increasingly suburban phenomenon. One theory suggests that the tick population is cyclical and this year’s numbers are so high (in our area, at least) because the rodent population thrived last year because we had such a bumper crop of acorns, etc. the year before that. Any thoughts on the validity of these ideas?
Hi Amanda,
Thanks for your message! I’m not sure that rodent are the primary carrier, but you are absolutely right that they can carry the Ixodes tick and are absolutely contributing to the tick/Lyme problem we are having. The trails around me have rodent traps for that very reason!
Sincerely,
Elisa
Back in November I had the classic bullseye rash on my righ calf. It took a full month to go away. No other symptoms have developed. I went to the doctor, she did a test where one marker came back positive but nothing else. She sent it for western blot, nothing. No antibiotics was prescribed. Do you think this is something I should look out for in the future? I found it interesting that I have had no symptoms other than the rash.
Hi there – that is very interesting. Many doctors would treat a bullseye rash without even checking a western blot as it’s pathognomonic for Lyme disease. But, if your immune system is strong, it’s very possible that your body can deal with Lyme or other infections effectively even without antibiotics. That would be awesome, and I hope that’s the case for you! I just would be aware that if unusual symptoms develop in the future, it may be nothing, but I personally would want to get tested for Lyme just in case a reactivation occurs.
Best to you!
Elisa
Thanks for a great article! I’m going to share this with my community.
I know this article is more about prevention and what to do right after a bite but because you’re so knowledgeable on this topic I’m curious what you feel about the new testing that Dr Klinghart is talking about for chronic Lyme detection and treatment (developed with radiologists Dr. Marco Ruggiero). I heard him share this on the upcoming Chronic Lyme Summit II: “we have set up a certain sequence of using ultrasound on the brain, on the thymus, on the spleen, on the vagus nerve, and on the brain stem. We drive out the microbes, and then we collect the urine and find the microbes. This is by far the best test we use – the PCR testing – looking for whole strands of DNA of the bugs in the urine.”
In this same interview he says “Most of my patients with severe, persistent Lyme disease have never had a tick bite. They had a spider bite or a flea bite or a bite from a stinging fly. So these are insect-borne diseases but not tick-borne diseases.” This is a scary thought and I’d love to hear your thoughts and what you see with patients.
I don’t work with clients to address their Lyme disease but refer out instead. However I do like to be well informed so they can get them the best help there is. While they are working with a Lyme literate doctor I am supporting their Lyme anxiety with GABA, theanine and tryptophan and diet so SSRIS and benzodiazepines don’t have to be added into the mix.
Thanks!
Hi Trudy,
I’m not sure that I agree that most patients have never had a tick bite. Mosquitoes have been found to be vectors, so I’m sure that other insects could be vectors as well, although I haven’t seen any confirmation of this in the literature. On the other hand, most people have no recollection of a tick bite because they are so small and often go undetected, and many never develop the classic bullseye rash. I think Dr. Klinghardt is brilliant, though, and his detection methods for chronic infections is absolutely cutting edge and beyond what most practitioners can do or are even aware of. It will be fascinating to see if his ultrasound provocation method will help us to identify the likely thousands of patients who have Lyme and other chronic infections that are going undiagnosed. And in the meantime, for patients who are suffering without or without a diagnosis, targeted amino acid therapy and dietary interventions that you do with clients is absolutely critical to restoring balance and harmony to their systems so that they can more effectively handle the psycho emotional stress of their illness AND their immune systems can more effectively fight their infections. So grateful for the work you do!
Sincerely,
Elisa
Thanks for the feedback and good point about the size of the ticks and no bulls-eye rash
I have 2 follow on questions
1) I appreciate that you are opposed to DEET and recommend essential oils but you do mention permethrin-treated clothing too. Do you have any concerns about toxicity?
2)I know you are assessing for and treating pyroluria (a social anxiety condition for readers here who may not be familiar with it.) Dr Klinghardt feels Lyme disease cannot be successfully treated until pyroluria is addressed. I’m curious if you’ve seen a connection?
Hi Trudy! I do have concerns about permethrin toxicity, but if you’ll be in a tick-infested area for a prolonged period, I think that wearing a light t-shirt and then having a permethrin-treated outer layer may be reasonable. And yes, I definitely see a connection with pyroluria and not just Lyme but any infection that can cause PANDAS/PANS. I don’t know what comes first though – if a chronic infection triggers metabolic imbalance with subsequent pyroluria, if or pyroluria sets the stage for immmune imbalance and subsequent chronic infection. But yes, both need to be treated simultaneously if present…
Take care!
Elisa
I loved your article THANK YOU! I am having a difficult Mom moment. I am working with LLMD’s as I’m recovering from Lyme, Bartonella and a parasitic infection. I’ve been almost bedridden for 6 months.
My almost 15-year-old only child went to Boy Scout camp this week in an area of Oklahoma where my husband and I were a bit repeatedly by ticks 18 years ago. There are so many there! I’m trying to be a good mom and not to deprive him of his childhood or make him absorb my paranoia. We armed him with all the right tweezers, tape rollers, alcohol, Ziploc baggies and powerful sprays to keep them at bay. He called home today homesick and after four days of backpacking in the mountains there he told us he had been bitten by at least 10 or more that had attached. They were small. Too small to save he said as they were squished when he pulled them out. He found them the same day and checked as diligently as any 14-year-old boy would. He will be home Saturday for two weeks before he takes a two week backpacking trip in the mountains of New Mexico with my husband that is a lifelong dream of his. I was prepared for a bite but not this many! He is not having any symptoms or illness but I feel the need to treat regardless for 3 to 4 weeks. The question is what with? I don’t want him sick for his New Mexico trip and I’m not sure what is the best thing to treat him with? Can you treat teenagers with Doxy? Does it cause sun sensitivity? None of my LLMD’s take insurance and all are hugely expensive. I could make a “antibiotic” of essential oil in a vegetarian capsule? I’m trying not to have a nervous breakdown. Thanks in advance for any advice.
Oh Shari – what a difficult place to be in! I totally hear where you’re at, and I would definitely be flipping out a bit, too! I guess it really depends on how healthy your son is at baseline, because not everyone who gets bitten by a tick that carries Lyme will actually get Lyme. But I know it’s especially frightening for you because you are experiencing the horrors of chronic Lyme disease firsthand. While I can’t give you specific medical advice for your son, if he were my child, I would give Amox and Azithromycin for 3 weeks and watch closely for any suspicious symptoms. I would not give my child Doxy because of the sun sensitization. Best wishes to you and your son, and I hope that you find recovery and healing soon!
xo Elisa
My son was bitten by a tick about a year ago and his lymph nodes in his armpit swelled up immediately. I gave him Biocidin for a month and after one dose his lymph nodes returned to normal. He exhibited no other symptoms so that was all we did. Then a few months later he said his arms hurt. I immediately thought Lyme and took him to a naturopath who found a whole list of coinfections along with Lyme which she is treating with Dragon Pearls formula. My question is when does the window close on giving antibiotics. Would it be too late now? He is not exhibiting any symptoms so I’m hesitant to go that route.
Thanks!
Hi Angela,
Tough question. There really isn’t a window that closes for using antibiotics. But if a child doesn’t have symptoms and is doing well, then making sure to keep the immune system and gut strong and healthy is really the best way to make sure that whatever infections are present remain in remission.
Good luck!
Elisa
Appreciate the call-out of Oil of Lemon Eucalyptus repellent products as a deet-free alternative. Healthy non-toxic tick & mosquito repellents safe for kids and pets – good tip to re-apply often. Our Cape Cod All Natural products are available at the National Seashore Store and registered with the CDC and select retailers and farmers markets and now Online.
capecodnaturals.com
thanks for the info! 🙂 Elisa
An excellent and thorough article! My son contracted Lyme seven years ago when he was ten. His Lyme-literate doctor put him on doxycycline for three weeks. In your article you say that “Doxycycline should not be given to children…”. I don’t dispute that. New information comes in all the time and seven years was quite awhile ago! My question is why? What did it do to his little body and are the effects lasting? Thank you for your time.
Hi Tami,
Thanks so much! So, doxy theoretically shouldn’t be given to kids under 8 years of age because of the possible effects on cartilage and permanent teeth staining. But you’re absolutely right – there’s always new knowledge, and it looks as though those concerns are largely theoretical and I have fewer concerns about using doxy than I used to, even at younger ages!
xo Elisa
I’m not sure I agree with the use of antibiotics since, in my understanding, the bacteria bind together in a bundle and are untouchable by antibiotics.
Also, I’m not sure using store-bought, canned, fermented foods are of any use because they have killed all the beneficial bacteria through the canning.
Hi Theresa,
For chronic Lyme, the organisms often live in biofilms and promote immune system activation of the coagulation cascade, so a biofilm and clot-busting protocol needs to be in place in order for any antimicrobial, whether pharmaceutical or herbal, to reach the spirochetes. For a recent tick bite, though, there should not really be a biofilm or hypercoagulability issue, so antimicrobials alone should be effective. And yes, home-fermented foods would be awesome ideally. But in the meantime, there are several companies that are now making great store-bought fermented options.
Thanks so much for your thoughtful comments!
Elisa
Hello, I am amazed that you take the time to reply to everyone. Thank you for that! My 3 year old was just bit and we lost the tick while wrestling him to get it out (he was not happy!). I don’t know what kind it was. Either way his pediatrician won’t give him antibiotics. I was planning to do that for him as well as ledum and arsenicum album. Then I was told on a Lyme Facebook group that ledum can damage the organs of children. Do you know this to be true. It’s so hard to know who to believe and what resources to trust! Thanks for your help.
Hi Bailey,
You’re so welcome! Homeopathic medicines, if appropriately dilute, should cause no damage on the organs. For instance, if I were to give my child Ledum 30C and Arsenicum album 30C after a tick bite, I would feel totally comfortable that there would be no side effects. If it were my child, I would also look into the herbal protocols by Stephen Buhner, which do not require a physician’s prescription.
Best to you and your 3-year old!
xo Elisa
My kid got bit Sunday.. we think and it is Tuesday night.. we just saw the bulls eye on his shin..
Is this an immediate doctor visit in the morning ? does this mean the Tick is in him?
What do we need to do?
Hi Josh. While I can’t give specific medical advice on what to do, yes! I would bring your son if to his doctor immediately. If it were my son, thn my approach would be to get on some sort of antimicrobial regimen ASAP – early treatment can absolutely prevent the progression to chronic Lyme disease. Best of luck to your son!
xo Elisa
My son is 7 years old (so too young for Doxycycline), weighs 25kg, and was prescribed amoxicillin, at a dose of 1200 mg/day (400 mg, 3 times a day), for 21 days. He had a bulls-eye rash, but no other symptoms that I have noticed. He began the antibiotics the day after I noticed the bulls-eye rash. His rash is fading, and looks like a small bump now.
I wanted to know if 3 weeks of antibiotics is long enough? Or does he need longer treatment?
At the end of antibiotic treatment, does he need to be seen by a doctor?
Hi Dianna – I’m so sorry for my late reply. I would absolutely have your son seen by a Lyme-literate doctor to ensure that he has been adequately treated, but for acute Lyme like what you’re describing, 3 weeks of Doxy should be fine!
Thank you Dr. Song for your thoughtful sharing of knowledge. My 5 year old daughter and I camped in our Pacific Northwest old growth woods 14 days ago. I was not informed about ticks, at all, and only burned mosquito coils at our campsite. I knew of ticks growing up in the sage brush desserts of Eastern Washington but didn’t realize they were a problem, literally in our deer friendly back yard. My girl spent the day crawling under little branch forts left behind by other campers. The next day she had a deer tick attached to her hair line. I removed it, applied iodine and was happy to see the small lesion heal up, but relieved when I read on the CDC site, that only 2% of tick bites result in Lyme. Tonight when putting her to bed my husband and I both noticed a 2 cm solid dark red spot at the bite site. I’ve been scouring the web for hours for information but am disheartened by the indication of Lyme if a spot or rash appears days or weeks after the bite. I am so thankful that her doc is a pediatric ND in Portland. I will share with her your site before seeing her ASAP. I hope for a complete eradication of the disease following her treatment plan which I’m sure will involve antibiotics + supporting medicines. I will be following your recommended diet instructions to balance her gut with the long course of antibiotics that seems inevitable.
I’m so sorry for my late reply! I’m hoping for the best for your daughter! You’re rapid action has most certainly helped her to thrive and be well! 🙂
Thanks for the tips on what to do when a person gets bitten by a tick. It got me when you said that we shouldn’t use caustic substances and get it lit because it will just make it worse. I will keep this in mind since I just found out that one of the trees in our backyard has ticks already. I was fixing our outdoor furniture when I saw some of these pests in it which made me really worried because our child might get bitten and get a disease. This tip will help me do the right procedures if ever.
You’re welcome, Millie! Hopefully you won’t have to use these tips! 🙂
Hi Dr. Song, I know this is an old post but we are in a bad way right now with my amazing 5yo son and I’m seeking help. He has tested for reactive 23, 41, 93 bands and is showing neuro /inflammatory symptoms of a bite that happened possibly 10 months ago. My big question for you.. is it too late for antibiotic treatment if it happened 10 months ago? (of course addressing mito and methylation / gut support as well)
Hi Rebecca – I’m so sorry for what you and your son are going through. It’s never too late. Please do find a Lyme-literate doctor to guide your son’s treatment. Best of luck! xo
Dr. Song, this is an amazing article. Unfortunately I pulled a tick off my 14 month old this evening. It is a female adult deer tick and I will send for testing ASAP. It was attached for 30 minutes max, most likely less. I pulled it out, the little prongs on the head were attached and came out, no parts left in his leg, Tick is in tact. Small mark from attachment on his leg which will monitor. I am on Cape Cod, MA so terrible area. Planning on calling the doc in the am this happened at 5 PM.
Would you still suggest the antibiotics?
Thank you
So great that you caught it so quickly! From what you’re describing, the risk of Lyme transmission is very very very low. Give you’re in Cape Cod, though, I would definitely follow what your doc recommends. Good luck!
Hello Dr, Song,
My 6 years old was bitten by a tick 7 days ago; he is currently taking antibiotics (3 weeks) as tick was carrying Borrelia. This is the second time in the past 2 yeas that he was bitten and infected by Borrelia (the first time he was also treated with antibiotics and we have been checking the antibodies in his blood for almost 2 years now), My question is; does this second infection increases his chances of developing a chronic Lyme. Also, should I include Astragalus 500 mg in his treatment (or maybe the tincture would be safer for a six years old?)
Hi Iva – I’m so sorry you and your son have to go through this, but so great that you found the ticks so early on and were able to get prophylactic treatment in right away. A second tick bite should not increase his risk for infection. If I’m understanding correctly, your son has been given antibiotics to prevent Lyme and his antibodies are fine so he doesn’t have any evidence of have been infected with Lyme. So preventing Lyme with antibiotics does not increase the risk of developing chronic Lyme disease because you would have had to contract Lyme in the first place. Just because a tick that carries Lyme has bitten you does not mean you’ll get Lyme – as long as it’s removed in time and treated preventatively, which it sounds like you’ve done! I’m not sure that Astragalus would help in addition to the antibiotics – definitely something to ask your Lyme-literate doctor. xo
Thank you very much for your prompt response: we really appreciate your help since in our region (all countries of former Yugoslavia) Lyme awareness is quite poor and is really hard to find a Lyme literate specialist, especially pediatrician.
I apologize for being rather unclear in my explanation: the first time my son was bitten , we did not find a tick, we only noticed an erythema migrans on my son’s leg. His blood was positive on Borrellia and he was given the antibiotics (3 weeks). We were advised to check his blood periodically (during the 2 years period) to see if the antibodies are increasing/decreasing. So, I understood that my soon was diagnosed with Lyme already, but he is OK since the antibodies have been decreasing.
Seven days ago he was bitten again, we pulled the tick out of his ear, tested it, and my son was given the antibiotics during the first 24 hours. I worry that this potential infection might trigger something from the previous Lyme that he was diagnosed with.
I was thinking about Astragalus to make his immune system stronger while (or afterwards) he is on the antibiotics? Thank you once again for your response and a wonderful , very helpful article.
Klinghardt’s blog says,
“Stephen Buhner’s treatment recommendations for new tick bites:
Astragalus 3,000 mg daily for 30 days, then indefinitely decreasing that to 1,000mg per day.
Andrographis tincture + green clay. Mix the two ingredients together to make a paste and apply to the tick bite area, as a way to prevent an active infection.
Joette Calabrese’s treatment recommendations for new tick bites:
Ledum palustre 200C dosed every 3 hours for the first day, then decreasing to two times per day for one week. Then twice per week for one month and finally once per week for another month.
Aurum arsenicum 200C. Taken at the same time as Ledum, if the tick was discovered in the last few days.
Borrelia 30C or Lyme Nosode 30C. Used in cases of older bites in addition to the first two remedies.
Joette also recommends preserving the tick in 180 proof vodka, grain alcohol or brandy. Which can be later used to make an iso-phatic remedy in case the first three remedies do not work.“
I’d do both. Good luck!
Hi Elisa, I thoroughly am grateful for your comprehensive article and generous replies. I believe my 3 year old daughter was bitten by 2 about 6 weeks ago behind her ear. I The ticks were most likely not attached for long as there was no sign of them. My husband was the one to tell me they were tick bites as I am fairly ignorant to all of this until recently. I did use some ledum homeopathic upon noticing the bites and watched for any rash to develop. The bites healed very quickly with no rash and has been her happy and healthy self ever since. After reading your article, I am freaking out. . I should also say we are now permanently living in Grass Valley which is a wooded area. I know I you can’t give medical advice, but what would you do in our shoes? Antibiotics? Herbal protocol? Astragalus? I cringe about the use of antibiotics, but would do it in s heartbeat if necessary. Thank you kindly!!
Hi Nicole – I’m so sorry for your worry! By 6 weeks post tick-bite, if your daughter is having zero symptoms, I am much less worried. If she were my daughter and I had any concerns (low energy, headaches, body aches, just not acting totally well), I would check a complete Lyme Immunoblot bloodtest at a conventional lab like Quest or Labcorp as a first screen (I don’t recommend the “Lyme antibody screen with reflex to western blot”). But if she were totally fine, i would not do anything but support her with healthy food and love as usual! xo
Elisa, thanks a lot for your work!!! This is so kind of you to educate us. We have just moved to Switzerland where ticks are in huge numbers. Here you can bring tick to any pharmacy to be checked and results are available on line. Prevention wise, I haven’t seen any information better than in your article. I understood about Lyme but What is your view on encephalitis. They recommend here to get vaccinated against encephalitis. What is your view on that? Thanks again! I keep following your blog and Facebook page:)
Warm wishes
Hi Elena – thank you so much for your kind words! I have heard that ticks are a big problem in Switzerland. Unfortunately, I don’t know much about the encephalitis vaccine. In general when I look at vaccinations, I consider the risks for contracting the disease and its severity (encephalitis is never good), and the risks of the vaccine for that individual… If it were my kids, since we love the great outdoors and I have pulled ticks off both of my children, I would definitely consider the vaccination for this potentially devastating encephalitis for which there is no treatment. Best of luck! xo
Elisa ! Thank you very much for your quick response. Your opinion is very important for me.
You mention a couple manufacturers for herbal options for prophylactic treatment post bite – what specific products do you use? Would love to try this route (for an adult) before antibiotics for a recent bite. Thank you!
Hi Heather – which herbal formulas and dosage I recommend really depends on the child, but I do frequently use Researched Nutritionals’ BLt and Beyond Balance’s MC-BB-1. good luck! xo
Hello Dr Song,
Your information in this article has really helped my family over the past few days. We found a tick in my daughters hair on a Saturday. Removed it easily and fully intact and no engorgement. It was an American dog tick. We don’t think it was attached very long. We treated the area with tea tree oil and mailed the tick to UMASS. By Monday, she had a fever, chills, headache, terrible sore throat and tummy ache. We went to the pediatrician expressing Lyme concerns which were thought by her to not be the case. We asked for amoxicillian and started it that day and sent a culture away for strep. We are awaiting the results of both the culture and tick test. In the mean time, we are dealing with the fever, headaches and sore throat. We are suspecting a tick borne illness but honestly have no idea. Does amoxicillian treat only the Lyme or other Tick illnesses as well? Our homeopath doctor muscle tested her against Lyme and it was negative….it’s a stressful and scary waiting game at this point.
I’m so sorry for how stressful this must be! Amoxicillin is really just for Lyme. I’m hoping everything worked out, and so glad you were able to jump on things so quickly! xo
Thank you for posting this article! I’ve been on the natural health band wagon for a little over 12yrs. But had never had to deal with ticks until we moved to the Santa Cruz mountains 5yrs ago. One son has been bit multiple times, I’ve sent in a couple ticks for testing but not all. From a natural health standpoint i always thought to try to avoid antibiotics When possible so I’ve always just treated with essential oils and homeopathy and watched for further symptoms. Luckily he has never developed any symptoms. I’m wondering now though if it would be prudent to get him tested. he’s been bit twice in the past 3 months one of them had been attached for 48-36 hrs possibly.
Would you have him tested even with no symptoms?
Without any clinical symptoms of acute or chronic Lyme disease, I typically do not test my patients… Stay well!
I have a son who has been bit multiple times but has never shown any further symptoms. I’ve treated the bite sites with EOs and homeopathy.
Would you recommend getting him tested? If it came back positive would you still treat it with antibiotics?
This is definitely something to discuss with your son’s physician and if your son tests positive for active infection, I would refer him to a Lyme-literate doctor if he were my patients. Without any symptoms, there may be nothing recommended but to support his immune system. So many considerations as to if, when, and how to test your son. If he were my patient, I likely would only test if I had any suspicions that he was showing signs of active or chronic Lyme disease…
My 2 week old son had a tick attached to him last week. We sent it away for testing and it came back positive for Lyme’s. They said it was semi-engorged and attached about 16 hours. What are your thoughts on treatment for a newborn?
I would strongly consider consulting a Lyme-literate doctor for next best steps. Best wishes to your son and family!
Hi Dr. Song,
Thank you so much for your great article. Our very active 13 year old was bitten by a tick on our June vacation last year hiking in Utah at some point and after 21 dr appointments here in Texas, he was finally diag with a tick illness in the rickettsia family of RMSF by a Pedi ID dr. After 3 long months of extreme fatigue, nausea, & stomach pain he was put on doxy. He slowly improved but has never been “normal” or active & athletic again and has regressed since Jan despite our dr continuing to look into other illnesses. Our family is desperate to help him become well. We have begun googling tick drs. Could you point us in a direction to help?
I’m so sorry to hear this, and with your son and family the best. I would look at an ILADS-trained doctor (International Lyme and Associated Diseases Society). Best wishes! xo