
Flu hysteria has now transformed into coronavirus hysteria, and many of you have asked me how worried you should really be. News around COVID-19 has taken the world by storm and many of us are not sure whether to panic or stay calm. Addressing the Munich Security Conference on Feb 15, 2020, World Health Organization (WHO) Director-General Dr Tedros Adhanom Ghebreyesus said:
… we’re not just fighting an epidemic; we’re fighting an infodemic …
This is a time for facts, not fear.
This is a time for rationality, not rumours. (1)
I always say that knowledge is power, but in this case, because the world has never seen this particular coronavirus (which is why it’s called “novel”), we don’t know a whole lot. Scientists and researchers across the world are scrambling to learn more about COVID-19 and possible treatment and prevention strategies, and we are learning more every day. I have to admit that I’m more worried about COVID-19 than I was when Kenzi had the flu with a 105.5 fever. But when I get anxious about something, I try to dig in and get the facts. And that’s what I did – for days. So let me share with you the facts that I’ve uncovered so that we can all be calmly and rationally prepared for a COVID-19 pandemic if it occurs. What follows below is the most evidence-based research I could find to help us navigate these times with as much knowledge as possible. All references are at the end, and I will update as new developments arise. Be forewarned – this is a long article, but I wanted you to have all the information you need in one place, instead of the gazillions of sites and resources I ended up scouring and piecing together.
Let’s fight fear with FACTS!
What is COVID-19?
COVID-19 was first reported in Wuhan, China on December 31, 2019, which started out as an outbreak, has since become an epidemic, and may be set to become a pandemic.
Let’s clarify the terminology. An outbreak happens when a disease occurs in greater numbers than expected in a community, and can even be just one case. You can have outbreaks in different communities. An epidemic is an outbreak that spreads rapidly to many people. A pandemic is an epidemic of global proportions that has become widespread across several countries or continents.
COVID-19 is the name of the respiratory illness caused by the 2019 novel coronavirus that was first detected in Wuhan, China. You will also see it referred to as the 2019 Novel Coronavirus, 2019-nCoV, or SARS-coV-2. Coronaviruses are a large family of viruses that are named for the spikes on their surface that look like crowns (“corona” in Latin means crown). By now, I’m sure you’ve figured out that COVID-19 has nothing to do with the Corona beer that you may have enjoyed at some point with a lime wedge, although many people have searched Google for “Corona beer virus”. Coronaviruses can cause mild illness like the common cold, or more severe illness like we’ve seen with SARS (Severe Acute Respiratory Syndrome) or MERS (Middle East Respiratory Syndrome), and now COVID-19.
How many people actually have COVID-19?
**As of March 12, I have stopped tracking case numbers, and I suggest that you do the same. We know that numbers are increasing everyday, and is set to affect 40-70% of us by the time this pandemic has resolved. In a way, the actual numbers don’t really matter. What matters is that we know that COVID-19 is here, and that we do our best to stay calm & rationally prepared. I do not recommend checking numbers daily – that will only serve to heighten your anxiety.**
The number of COVID-19 cases and deaths are increasing every day, so these numbers are a moving target. As of March 11, 2020, the World Health Organization has officially announced that COVID-19 is a global pandemic.
I have been looking at the global Coronavirus COVID-19 tracker from Johns Hopkins for accurate daily numbers. which synthesizes data from 5 different sources: WHO, CDC, European Centre for Disease Prevention and Control, China’s National Health Commission, and ncov.dxy.cn, an independent data source maintained by Chinese physicians.
As of March 12, 2020, there have been at least 127,863 global confirmed cases, 80,932 of which are in mainland China. The rate of new daily cases in China is slowing down while the rate in other countries has been increasing. Italy, Iran, and South Korea have the next highest number of COVID-19 cases, at 12462, 10075, 7869 cases respectively. As of March 12, 2020, there are 1,323 cases of confirmed COVID-19 in the US.
Infection from exposure to COVID-19 from within the reporting country is far surpassing infection from exposure due to travel from another country, with an increasing number of infected persons with no history of international travel or close contact with a patient with known infection. Domestic community spread is becoming an increasing concern in the US and in other countries, and we need to have more strategies for early detection, containment and treatment than just closing our borders.
How is COVID-19 transmitted?
It is now clear that human-to-human transmission of COVID-19 is possible and is occurring. Transmission is mainly through respiratory droplets and close contact – similar to how influenza is spread. The CDC defines close contact as being within 6 feet or within a room or care area for a prolonged period without personal protective equipment OR having direct contact with secretions of a person with COVID-19 infection. There is some evidence that fecal-oral or blood transmission may be possible, even when COVID-19 is not detected in oral swabs (3).
SARS-CoV-2 is now known to survive on various surfaces and possibly be transmitted through “fomites” (a fancy word for objects or materials that can carry infection, such as tabletops, keyboards, clothes and utensils), and may also possibly have airborne transmission. This study (37) found the following survival rates on various surfaces:
- Aerosol (in the air) – at least 3 hours
- Copper – 8 hours
- Cardboard – 8 hours
- Stainless steel – 48 hours
- Plastic – 72 hours
The incubation period is thought to be 2-14 days, with a median incubation period of 4 days. Patients are thought to be most contagious when they are symptomatic. However, one report (4) found that an asymptomatic woman who transmitted COVID-19 to 5 other people may have had an incubation time of 19 days.
What are the symptoms of COVID-19?
What is important to remember is that the vast majority, likely over 80%, of infected people appear to have mild infections – with mild cold-like symptoms and fever, and likely many who have no symptoms. As noted above, there are case reports of asymptomatic carriers. However, most people who contract COVID-19 do seem to develop symptoms of some sort.
Reported symptoms include:
- Fever (which may not be present in the very young or very old, or immunocompromised)
- Uncomplicated upper respiratory symptoms (Cough, sore throat, nasal congestion, malaise, headache, muscle aches)
- Difficulty breathing
- Mild pneumonia
- Severe pneumonia (the severe pneumonia caused by COVID-19 is now named severe acute respiratory infection (SARI))
- Diarrhea and other GI symptoms (nausea, anorexia)
- Loss of smell (anosmia) and taste (ageusia)
- Acute Respiratory Distress Syndrome (ARDS)
- Sepsis and Septic shock
- Death
Death is of course what we are all worried about. So let’s look at that a little more closely in the next section.
What is interesting to note is that children seem less vulnerable to infection and appear to have milder symptoms than adults. There have been NO reported deaths in children 0-9 years of age. One very small study of 9 infants under 1 year of age infected with COVID-19 found that none of the infants had severe illness or complications. In fact, 1 had no symptoms, 2 had mild upper respiratory tract symptoms, and 4 had fever. (5) Another larger study (38) of 2143 pediatric patients (731 lab-confirmed and 1412 suspected), 94.1% had no to moderate symptoms. There was one death in a 14-year old child, and to date there have been no reported deaths in any child under 10 years of age.
Pregnant women also do not appear to be at greater risk for complications. In a small study of 9 women in Wuhan in their 3rd trimester of pregnancy with confirmed and symptomatic COVID-19 infection, none developed severe pneumonia or died. All gave birth via c-section to healthy-appearing babies with normal Apgar scores. No virus was found in amniotic fluid, cord blood, breastmilk or neonatal throat swab. (6) Two additional studies also confirmed that intrauterine infection does not occur, and reported no deaths in mothers or newborns. (39, 40)
What is the COVID-19 mortality rate?
Unfortunately, we don’t really know. As stated above, we need real case numbers to know real death rates. The high number of deaths in China is devastating, but may not be reflective of mortality rates in other parts of the world given the tragic lack of hospital staff, medical supplies, ICU beds, and test kits that China is facing. And this may similarly be the case in other countries like Iran.
If we just look at our current numbers, the death rate appears to be quite high. The reported mortality rate is highest in Italy at 10%, in China it is 4%. BUT – let’s take a look at South Korea. In South Korea, after testing 100s of thousands or people, the mortality rate is closer to 1.4% mortality rate – much lower than the 2-3.5% mortality rate that is currently being reported in the news. In an editorial written by Dr. Anthony Fauci, MD director of the National Institute of Allergy and Infectious Disease, he writes:
“If one assumes that the number of asymptomatic or minimally symptomatic cases is several times as high as the number of reported cases, the case fatality rate may be considerably less than 1%.” (33)
Note that even 1.4% is still significantly higher than the estimated 0.1% mortality rate from influenza. No death is to be taken lightly, and my heart goes out to those who are suffering tragic losses. But before we accept the high reported mortality rate and succumb to the rapidly worsening hysteria and potential worldwide economic collapse, we need REAL NUMBERS. I urge policymakers to quickly develop more widespread and rapidly available testing capabilities, not simply to quarantine those who are infected, but to shed real light on the gravity of the situation and help the public, clinicians, public health departments, and businesses be calmly and rationally prepared.
That being said, we certainly do not want to take any deaths lightly. Certain populations do seem to be more at risk for serious infection and for death. Increasing age seems to be the most important factor, and as mentioned above, children appear relatively spared. In a report released by the Chinese CCDC on February 17, 2020 in the Chinese Journal of Epidemiology, the risk of death increases with age, with being over 80 the highest risk factor. The fatality rate of patients over 80 years old was estimated to be 14.8%. Death in those under 50 appears to be unlikely, with the mortality rate of 40-49 year olds estimated to be 0.4% and 0.2% for patients 10-39 years of age. As noted above, there have been NO deaths in children 0-9 years old. Having a chronic, pre-existing medical condition also significantly increased the risk of death. Without any pre-existing condition, the mortality rate was 0.9%. A history of cardiovascular disease increased the risk to 10.5%. (7)
So like the influenza virus, the elderly and those with underlying chronic medical conditions appear to be most at risk for serious complications and death from COVID-19. However, unlike influenza, children so far appear to be relatively protected.
How and who do you test for COVID-19?
COVID-19 is detected by testing nasopharyngeal swabs (basically a q-tip up the nose), oropharyngeal swabs (a throat swab), and sputum for genetic material of COVID-19 by polymerase chain testing (PCR). The test kit is called the “Centers for Disease Control and Prevention (CDC) 2019-Novel Coronavirus (2019-nCoV) Real-Time Reverse Transcriptase (RT)-PCR Diagnostic Panel.” In the US, these test kits are NOT widely available currently through doctor’s offices, community clinics, or hospitals (i.e. I do NOT have test kits). The CDC has begun rolling out test kits to certain state public health departments, including California and hospital labs and commercial labs like Quest and Labcorp have already rolled out their testing. BUT, there are still not enough testkits to test every patient with fever and upper respiratory symptoms. There are not enough nasal swabs and “V-C-M” media for community clinicians like me to test possible cases, and sending nasal swabs to Quest or Labcorp have the further difficulty of needing to be sent on ice.
Currently, the recommendations are to test patients with fever and lower respiratory symptoms (cough or shortness of breath) who have had close contact with: 1) a person with confirmed COVID-19; or 2) history of travel from affected geographic areas with 4 days of symptoms; OR anyone with severe acute lower respiratory illness that requires hospitalization and does not have another diagnosis like influenza, even without any known source of exposure. Remember, the CDC defines close contact as being within 6 feet or within a room or care area for a prolonged period without personal protective equipment OR having direct contact with secretions of a person with COVID-19 infection.
This is the protocol that was emailed to me by my local health department (8):
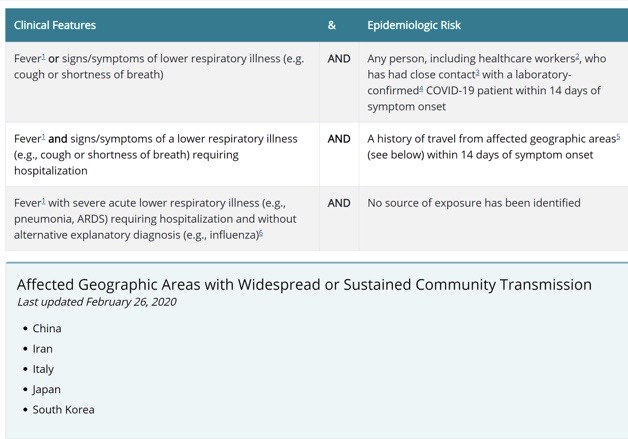
The CDC also recommends that providers test for other respiratory pathogens, like they would as part of their usual workup for anyone who comes in with fever, runny nose, and cough – like the flu! Because let’s face it, we’re still in the middle of flu season, and …
If you or your child have cold or flu symptoms,
there is a good chance that your child has a cold or the flu!
As we begin to see more domestic spread of COVID-19 in the United States, please …
Do NOT rush to your doctor’s office or hospital to get tested at the first sign of fever or cough unless your health is declining and you need urgent medical attention.
Your doctor or emergency department likely has very limited capability to test for COVID-19, and going unnecessarily to the doctor’s office or emergency department may inadvertently expose you or your child to COVID-19 or other infections and likewise expose other people to whatever illness you may have. Many cases of COVID-19 in China are likely due to uninfected people becoming infected after exposure while waiting in long hospital and clinic lines to be tested. The California Department of Public Health urges that:
If a person develops symptoms in COVID-19 including fever, cough or shortness of breath, and has reason to believe they may have been exposed, they should call their health care provider or local health department before seeking care. Contacting them in advance will make sure that people can get the care they need without putting others at risk.
How do you treat COVID-19?
There are currently NO specific antiviral medications known to treat COVID-19, Treatment is supportive with rest, fluids, oxygen, and more intensive care if needed. Scientists are actively researching possible existing or new antiviral medications that may have activity against COVID-19, and vaccines that may help to prevent COVID-19. Tamiflu will not work. While these efforts are critically needed, the manufacture and testing of a new pharmaceutical agents or vaccines is likely several months to over a year in coming.
There are currently over 80 clinical trials across the world looking at pharmaceutical and even natural treatment options for COVID-19, including high-dose Vitamin C. Hydroxychloroquine, a safer version of chloroquine, appears to hold the most promise. A study in Marseille (41) found that a combination of hydroxychloroquine of 300mg TID x 10 days + azithromycin 500mg on Day #1 then 250mg QD on Days #2-5 significantly reduced viral load and percentage of patients still carrying SARS-CoV-2 at 6 days.
Other potentially promising medications under investigation are Remdesivir, Sarilumab (a human IL-6 receptor blocking monoclonal antibody), and anti-SARS-CoV-2 IgG antibodies from infected patients.
In the meantime, while there are no pharmaceutical options approved for COVID-19, are there any existing natural treatments that might work? We just don’t know. A huge amount of funding has been committed to clinical treatment trials. While we wait anxiously for results, I urge scientists and researchers to consider some of the evidence we currently have about natural treatments for prior coronavirus outbreaks (SARS, MERS) and sepsis that may theoretically hold promise for successfully treating COVID-19, and would be more readily available and much less costly than any newly-engineered drug.
I am here to educate and inform, NOT to recommend any particular treatments because we simply do not yet know what will be effective against COVID-19. I did this research out of an effort to educate myself on all possible therapeutic options if/when COVID-19 arrives. Here is what I found. These are theoretical possibilities only. Please do not stockpile these natural medicines. If you suspect you or your child has COVID-19, please consult with your physician on your best treatment options.
Zinc has been found to inhibit Coronavirus RNA polymerase activity in vitro and zinc ionophores CAN block the replication of these viruses in cell culture. (42) Zinc + zinc ionophores (compounds that affect the cellular transporters for zinc) have been shown to block SARS-CoV multiplication, which means that they may be able to stop the current circulating SARS-CoV-2 from replication and wreaking havoc in our immune systems. (43) What’s fascinating is that chloroquine is a zinc ionophore, and this (44), and this maybe why it has been found to be helpful in Coronavirus infection.
Quercetin and Epigallocatechin-gallate (EGCG found in green tea) have also been found to have zinc ionophore activity (45), and should therefore be considered for research in all potential treatment options for COVID-19.
Sambucus Formosana Nakai (a species of elderberry similar to Sambucus nigra or black elderberry that has been found to have anti-influenza activity) was found to have strong activity against Human coronavirus NL63 (HCoV-NL63). (9) NOTE: This is NOT the same as the elderberry syrup you’ll find on shelves, and I am not recommending that you go out and stockpile Sambucus Nigra). The caffeic acid component of Sambucus Formosana Nakai seemed to be responsible for most of the anti-HCoV-NL63 activity, and significantly inhibited replication and blocked attachment of HCoV-NL63. Caffeic acid is actually NOT related to caffeine, but is found in many foods such as coffee, wine, turmeric, basil, thyme, oregano, sage, cabbage, apples, strawberries, cauliflower, radishes, mushrooms, kale, pears, and olive oil. It definitely couldn’t hurt to load up on caffeic acid-rich foods (minus the coffee and wine, perhaps…). [PLEASE NOTE: I have been asked where people can find Sambucus Formosana Nakai, and unfortunately, as far as I can tell it is not available commercially. I included this information for research purposes, and do not know if Sambucus nigra would have similar effects.]
Traditional Chinese Medicines have been met with significant controversy and panic stockpiling when Chinese researchers claimed that a traditional herbal formula (shuanghuanglian made with honeysuckle, Chinese skullcap and forsythia) could inhibit 2019-nCoV in vitro. This was a premature announcement and clinical trials need to be performed. However, if we look to prior research on other coronaviruses, there are studies showing the efficacy of various Chinese herbal agents against other coronaviruses, including SARS-CoV and CHOV-22E9. (10) These herbal medicines include: Bupleurum, Heteromorpha, and Scrophularia scorodonia (11); Lycoris radiata, Artemisia annua, Pyrrosia lingua, and Lindera aggregata (12); Isatis indigotica and Torreya mucifera (13,14,15); and Houttuynia cordata (16) My hope is that researchers take interest in these initial in-vitro results and consider clinical trials that could potentially find a cure in these natural agents.
COVID-19, sepsis & cytokine storm
When patients with COVID-19 die, it is often due to sepsis, in which the immune system goes haywire and overreacts in what is called a “cytokine storm.” Natural agents that are immunomodulatory and immunoregulatory, and bring BALANCE to an overactive immune system, may be one of the best options to support patients with sepsis. Here’s what the literature shows for what may be helpful for critically ill patients with sepsis. In life-or-death critical situations like sepsis where conventional medicine does not offer significant success, I would urge researchers to consider all potential treatment options for further investigation.
Vitamin C, 1.5 grams IV every 6 hours (6 grams total daily), given with hydrocortisone and thiamine was found to significantly decrease mortality and prevent progressive organ failure in patients with sepsis. In fact, patients treated with the vitamin C protocol had an 8.5% death rate compared with 40.4% in the control group! (17) Thankfully, there is currently a research trial underway to investigate vitamin C infusions for the treatment of severe 2019-nCoV infected pneumonia (18) where patients in the treatment group will receive 24 grams of Vitamin C daily for 7 days.
Vitamin D has been called a “pro-survival molecule.” In this review of the literature on Vitamin D and immunity (19), the authors conclude that:
“… vitamin D not only helps the immune system to be dampened during an excessive or chronic reaction (anti-inflammatory potential) but also to rapidly reach its completion or exhaustion, helping innate cells to kill bacteria or viruses. In this sense, vitamin D maintains its pivotal role as a pro-survival molecule.”
Cathelicidin produced by Vitamin D can neutralize LPS (lipopolysaccharides) that are responsible for so much of the damage that we see in sepsis, and also has antimicrobial and immunomodulatory effects. (20) Vitamin D deficiency may actually be considered a risk factor for sepsis and inflammatory disorders, so please ensure that your and your child’s vitamin D levels are optimized as I discuss below in how to protect your child.
Other Natural Agents: This journal article from 2014, Therapeutic interventions in sepsis: current and anticipated pharmacological agents by Shukla P, et al (21), is probably the best article I’ve found on evidence-based yet outside-the-box thinking of potential natural treatment options for sepsis that warrant further investigation. Here are just a few of the fascinating findings:
- Curcumin has been found to inhibit NF-kB – potent activator of inflammation in sepsis. Curcumin was also found to inhibit binding of LPS and suppress the LPS-induced inflammatory response and damage seen in sepsis, while improving survival, in a mouse model of sepsis. (22)
- Quercetin has also been found to inhibit the NF-kB pathway (23), and to improve survival and decrease cellular damage in a mouse model of sepsis (24,25)
- Naringin, a flavonoid found in the skin of citrus fruit, ameliorated LPS-induced sepsis in mice, via the NF-κB pathway, and reduced LPS-induced acute lung injury (26)
- The probiotic Bacillus sp strain LBP32 has extracellular polysaccharides (EPS) that were found to inhibit the LPS-induced release of many pro-inflammatory mediators (such as NO, ROS, IL-6 and TNF-α) by inhibiting the NF-κB pathway. Researchers were able to demonstrate that EPS could greatly improve the outcome of mice with LPS-induced endotoxic shock (27). [Please note: this particular Bacillus strain is not available commercially that I can find. I included it for research purposes. I do not know if other strains would have similar benefit but we do know that probiotics have amazing immune supporting properties in general…]
- Boswellia (Frankincense) can inhibit LPS-induced inflammation in sepsis. This study (28) found that Casperome® (Casp), an orally bioavailable soy lecithin-based formulation of standardized frankincense extract, was able to ameliorate the systemic effect and multi-organ damage induced by severe systemic inflammation using a mouse model of sepsis.
- Lomatium dissectum is a Native American traditional root that was claimed to have prevented the Washoe Indian tribes from dying during the 1918 influenza pandemic (also called the Spanish flu pandemic). In SARS-CoV sepsis, one of the inflammatory chemokines involved is CXCL10 (29). Poor prognosis with Influenza A is also associated with CXCL10 dysregulation. Lomation dissectum, used by Native Americans in Western US to treat influenza, was found to inhibit CXCL10 secretion by lung cells and may explain why during the 1918 influenza pandemic, L. dissectum was hailed as the cure for influenza and influenza-associated pneumonia. (30)
Is airplane travel safe right now?
As we see more outbreaks in countries outside of China, the CDC has added several countries to its travel advisories, with “most” of Europe being the most recent. The alerts below are as of March 12, 2020:
- Level 3: Widespread sustained (ongoing) spread and restrictions on entry to the US – Avoid all nonessential travel, and entry of forein nationals have been suspended from China, Iran, and most of Europe.
- Level 3: Widespread sustained (ongoing) spread – Avoid all nonessential travel to South Korea.
- Level 2: Sustained (ongoing) community spread – Special precautions for high-risk travelers. Older adults or those with chronic medical conditions should consider postponing travel to any destination with an outbreak.
Travel advisories are a moving target, and as I write, “most of Europe” was just added to the list. If you are planning international travel, keep informed with the CDC’s COVID-19 geographic risk assessment page. Whether you choose to travel or cancel any upcoming plans is a completely personal decision, and I cannot recommend you choose one path or another. I personally am limiting international travel for me and my family. While I am lucky to have a busy domestic travel schedule teaching integrative and pediatric functional medicine to other practitioners, if given the choice, I would limit even my domestic travel until we know more. I am much less concerned about the risk to me and my family as I am about the risk of my family contributing to the spread of COVID-19 to vulnerable populations. We all have to make whatever decisions we feel most comfortable with for our families, but if you are planning air travel, please read my airplane travel tips and tricks that I list in my blog post How to Have a Healthy, Happy Holiday.
How can you protect your family from COVID-19?
Remember, the vast majority of people appear to have mild illness, especially children. Researchers are investigating what makes certain populations more vulnerable to severe illness. However, we know from other viral illnesses that there are ways to reduce our susceptibilities to serious illness.
Infection + Susceptibility = Symptoms
If we can reduce our individual susceptibility to serious illness, our likelihood of developing mild symptoms if we are infected is much higher. So let’s take a look at some of the possible ways that we can reduce our susceptibilities to protect our families.
There are commonsense measures to protect yourself from COVID-19 that you should be practicing regardless of whatever virus is circulating at the moment. The only unique recommendation with COVID-19 is to avoid unnecessary contact with non-domesticated animals due to presumed animal-human transmission. Other commonsense measures to protect yourself and prevent spread of illness include:
- Wash hands frequently, especially before eating or touching your face. Washing hands with warm soap and water for at least 30 seconds is the best option. This study found that washing hands even with plain running water without soap was more effective than ethanol-based hand disinfectants at killing the Influenza A virus! (31) But you have to wash your hands the RIGHT WAY! Be sure to read my article Handwashing & Coronavirus: Are you doing it the right way? to teach your kids (and yourself!) how to do it correctly.
- Use a hand sanitizer with at least 60% alcohol. If you don’t have access to soap ad water, an alcohol-based hand sanitizer is the next best thing. But it has to be at least 60% – this is the percentage found to kill coronavirus in studies (36). With the run on Purell, you may need to make your own – but you have to make it the RIGHT WAY to have coronavirus-killing effects. Read my article for recipes on How to Make Your Own 60% Alcohol-Based Hand Sanitizer.
- Avoid touching your eyes, nose, and mouth! Do your best to keep those little fingers away! The first step is helping children (and adults) be mindful how how often we actually do touch our faces! Varying studies have shown that we touch our faces on average 23-50 times per hours. So help your children notice when they’re touching their faces so they can pay attention to not touching their faces even when you’re not with them. And instead of nagging them to “Stop touching your face!”, focus on the positive and what they CAN do, not what they shouldn’t. Try “Keep your hands down” for a change.
- Stay home when you’re sick, unless you need urgent medical attention. You may be increasing your possible exposures to COVID-19 if you don’t have it, or exposing others unnecessarily if you do.
- Cover your cough with your elbow or tissues. Teach your kids proper cough etiquette. And if you use a tissue, immediately throw it into the trash and wash your hands.
- Keep your distance. Try to stay at least 6 feet away from anyone who is obviously sick with fever and/or respiratory symptoms.
- Irrigate your nose. While we do not know if nasal irrigation makes a difference for prevention of COVID-19, I believe that one of the MOST preventive things you can do for any viral respiratory illness is to irrigate your, and your children’s, nasal passages with saline or Xlear nasal spray at the end of every day and after any potential exposure (work, school, playgroups, plane travel, etc.). One study found that people who did preventive daily nasal irrigation had significantly fewer episodes of upper respiratory symptoms, shorter symptom duration and fewer days with nasal symptoms compared to those who did not irrigate their nose daily (34). Xlear is a saline nasal spray with xylitol and grapefruit seed extract, both of which have antimicrobial properties. You cannot overdo it, and will not get “addicted” to it. Other options for nasal irrigation are a regular saline spray, Neti pot, and other sinus rinses like Neilmed.
**Apart from regular hand washing, I believe that daily and frequent nasal irrigation is one of the MOST important things that we can do to prevent influenza and other viral respiratory infections from taking hold.** This is because after exposure to a virus, the influenza virus tries to invade and multiply in your nasal passages for at least 1-2 days before you develop any symptoms. Nasal irrigation can wash away viral particles before they have the opportunity to take hold, and thereby prevent many infections from happening in the first place! - Load up on foods and spices with antiviral properties. These include coconut oil, raw garlic, oregano, ginger, kimchi and other fermented foods, walnut, pomegranate, green tea, apple cider vinegar, and medicinal mushrooms (shiitake, maitake, reishi, cordyceps, turkeytail).
- Eat lots of colorful fruits and vegetables. They are full of antioxidants which will destroy the free radicals that weaken our immune system and are responsible for making us feel sick when we catch a bug. Each color provides different antioxidant power – so be sure to eat a rainbow every day. If your kids aren’t the hugest vegetable eaters yet, give them their antioxidant dose with a smoothie packed with fruits AND veggies, use that smoothie to make jello with grass-fed gelatin or popsicles, sneak pureed vegetables into your spaghtetti sauce, soups, chilis, or whatever other way you can think of – be creative!
- Stay well-hydrated. Stick to water, coconut water, herbal teas, and bone broth. No soda or sugary drinks, please! What’s a good estimate for how much water you need at a minimum? Divide your body weight (in pounds) in half and drink that number in ounces! Do you come close?
- Drink your bone broth! Bone broth has amazing immune-supporting properties. See Amazing Bone Broth to get started easily making your own.
- Eat fermented foods. The probiotics contained in fermented foods have tremendous immune boosting powers. In fact, the fermented Korean cabbage, kimchi, was found to have significant effects in preventing and fighting the H1N1 influenza virus! Other examples of delicious fermented foods to try include sauerkraut, pickles (try “real” pickles without added vinegar like Bubbies), miso, kefir, and kombucha.
- Avoid simple sugars and processed/junk food. Did you know that your blood shows lab evidence of a lowered immune system within 30 minutes of eating simple sugars (like glucose, refined sugar, and fructose), and causes a 50% reduction in your white blood cells’ abilities to kill germ? (35) White blood cells are our “army” cells that fight off germs. This effect is most noticeable 2 hours after ingestion, but is still present 5 hours later! Keeping blood sugar levels healthy has been shown to improve immune system activity.
- Get fresh air and moderate daily exercise. Moderate exercise can boost the production of macrophages, the kind of white blood cells that “eat” bacteria and viruses. However, intense exercise can actually temporarily decrease immune function – so don’t overdo it!
- Get adequate sleep. An increase in sleep actually increases the number of your white blood cells. On the other hand, loss of sleep even for a few hours at night, increases inflammation in our body which makes us more susceptible to catching the flu and having more severe symptoms. So make sure your whole family is getting enough zzzz’s. For tips on getting a good night’s sleep, see Eat Yourself to a Good Night’s Sleep and The 3 Things You Need to Know to Get a Good Night’s Sleep.
- Minimize stress. Emotional stress creates physiological stress in our bodies that lowers our immune defenses and makes us more vulnerable to illness. Stress has been shown to lower our white blood cells’ abilities to kill germs, and actually creates more inflammation that may make us feel even sicker. For guidance on how to help manage your child’s stress naturally, take a look at my articles 6 Steps for a Stress-Proof Child and Mindfulness for Kids for some great tips.
Should I wear a mask?

Face masks are currently not recommended for the general public. They are only recommended if you have a cough that you could transmit, or are taking care of someone who is sick with COVID-19.
That being said, this new research paper from February 19, 2020 that has yet to be published (32) compared medical staff at Zhongnan Hospital caring for patients with COVID-19 between Jan 2-22 who were medical staff in the Respiratory, ICU and Infectious Disease Departments and wore N95 respirators and washed hands frequently vs. medical staff in the Hepatobiliary Pancreatic Surgery, Trauma and Microsurgery and Urology Departments who who wore no masks and disinfected their hands less frequently. Even though the masked group actually encountered more confirmed cases of COVID-19 than the unmasked (730% MORE cases, in fact), none of of the 280 staff contracted 2019-nCoV. On the other hand, 10 of the unmasked group became infected.
So, if the pandemic starts to hit a little too close to home, will I be wearing a mask and make Peter, Kenzi and Bodi wear one? Probably yes! If you do wear a face mask, please make sure it’s a “Particulate Respirator Mask” that filters at least 95% of very small particles and is marked P95, R95 or N95, has 2 straps, and forms a tight seal around your nose and mouth. A regular surgical mask will provide no protection and is actually meant to protect others from your cough or sneeze. A properly fitted respirator mask should be worn over BOTH the nose and mouth, and form a tight seal so that you can’t smell any ambient odors. A good test is to put on the mask covering your mouth and nose, pinch the mask across the bridge of your nose, then spray peppermint or lavender essential oil in front of your face. You should not be able to smell or taste any of the oil in your nose or mouth through the mask.
THE PROBLEMS: A major concern is the shortage of personal protective equipment (PPE) for our medical staff in the frontlines. Ensuring that our medical personnel who will be caring for our sickest patients have the proper gear to protect themselves is of utmost priority, so please – do not stockpile masks, and do your part to donate or make handsewn masks to protect our COVID-19 first resonders. Most masks won’t properly fit and create a good seal over a young child’s mouth and nose to filter out small smoke and air pollution particles, so make sure you follow the suggestions below for immune boosting. Remember, though, that preliminary reports seem to show that children are much more likely to have mild and even asymptomatic disease.
Keep your immune system as strong as possible.
Consider keeping your immune system even more supported with the following nutritional supplements to give your body even more antiviral defense:
- Fish oil – Omega-3 essential fatty acids have a host of immune benefits too long to list!
- Probiotics – One study showed a dramatic reduction in fever and upper respiratory symptoms in children who took a probiotic with a specific combination of Lactobacillus and Bifidobacterium daily throughout the cold and flu season. This particular combination of Lactobacillus and Bifidobacterium can be found in Metagenics Ultra Flora Children’s Chewable probiotic, Ultra Flora Synergy powder, and Ultra Flora Balance capsules. The recommended dosage for children and adults is ¼ tsp 2x/day, 1 capsule 2x/day, or 1 chew 2x/day. Probiotics are why fermented foods pack such a punch, so if your child’s palate hasn’t expanded yet to include a lot of fermented foods, be sure to give her a probiotic supplement to keep her gut and immune system healthy! If you want to know more about which probiotic supplement is right for your child, be sure to download my FREE Guide to Choosing Your Child’s Probiotic!
- Vitamin C – Vitamin C is a powerful antioxidant which assists our ability to ward off and deal with infection. Remember the vitamin C and sepsis study above? I have been using Metagenics Ultra-Potent C because it has added ingredients such as lysine and glutathione which assist in fighting viruses.
- Vitamin D3 – There is speculation that rates of illness increase over the winter because of the widespread deficiency of Vitamin D. As mentioned above, Vitamin D deficiency may be one of the risk factors for sepsis. Studies have shown that people supplemented with adequate levels of Vitamin D3 during the cold and flu season had significantly lower rates of infection. Vitamin D3 increases our body’s production of cathelicidin, an antimicrobial compound, to help fight viral and bacterial infections, that I discussed above in the section on sepsis. The Vitamin D Council recommends a maintenance dosage of 1000IU of Vitamin D3 per 25 pounds of body weight (the dosage may be higher in people with Vitamin D deficiency, which is epidemic and can be measured through an easy blood test). **Vitamin D3 is one of the supplements that I am “religious” about giving to my kids.**
-
Concern has been raised by some that Vitamin D3 may increase ACE2 receptor expression and worsen COVID-19, and should therefore be avoided. A similar concern was raised by the French Minister of Health when he rang the alarm bells that NSAID medications (like ibuprofen) may be a common risk factor in patients with severe illness and to use acetaminophen instead for symptom relief. The theoretical concern is that SARS-CoV-2 attaches to target cells via angiotensin-converting enzyme 2 (ACE2) receptors, and medications that increase ACE2 receptor expression may allow more SARS-CoV-2 particles to attach to lung cells and potentially lead to more invasive disease. Many have criticized these statements as premature, as there is evidence to the contrary that ACE2 supplementation may actually be beneficial in treating SARS-CoV and sepsis. And there are also many reasons to have concern for acetaminophen use, including the depletion of glutathione, our master antioxidant, which may prolong symptoms and increase infectivity. Read my article NSAIDS & Coronavirus: should we be worried?” for my full analysis. So for the moment, knowing that the vast majority of people are Vitamin D deficient or insufficient, and knowing how protective Vitamin D is for optimal immune system functioning, I continue to believe that Vitamin D3 supplementation is an important part of a Coronavirus immune support protocol.
-
- Zinc – Zinc is required for the normal functioning of white blood cells. Supplementing with just 15mg of zinc per day in adults has been found to improve our immune cells’ ability to ward off infection.
If you or your child does get sick…
If you DO start to feel a fever and cough coming on, remember – it is very likely the common cold, influenza, or one of the other more commonly circulating viruses and NOT COVID-19 – so DON’T PANIC. And even if it is COVID-19, remember that most people appear to have MILD symptoms. If I were concerned that I or my family had COVID-19, I would still use the same pediatrician-approved natural remedies for colds and flu-like illnesses that I detail in these 2 resources:
- My article Pediatrician-Approved Natural Remedies for the Flu
- My online course Everyday Holistic Pediatrics – the ONLY comprehensive online video course of pediatrician-designed, mama-approved natural remedies to boost your child’s immune system and get them through their fever, flu, cold, cough, earache, vomiting/diarrhea, sore throat and pinkeye using diet and lifestyle, homeopathy, herbs, essential oils, and acupressure!
As a disclaimer, I am not in any way recommending natural treatments as a replacement for standard medical care or vaccination, but until that time that effective medical treatments or vaccination for COVID-19 are developed and approved for use in kids and adults, I will be using all the tools I have that I know can work for other viral respiratory illnesses, like the flu. And you bet if Kenzi and Bodi get sick, I will be pulling out my vitamin D3, vitamin C, Windbreaker, Elderberry syrup and VClear, OnGuard or Thieves essential oil, and loading them up with antioxidant-rich foods. For an easy reference, you can download my FREE GUIDE: Natural Remedies to Beat the Flu! (This is for the flu, but may have relevance for COVID-19).
Phew – there you have it. Everything I’ve learned so far and want you to know about COVID-19, and everything I intend to do for my family, from a holistic pediatrician’s perspective. We will continue to learn as more research is done, and I’ll be sure to update this post to share everything I know so make sure you’re signed up for my newsletter to be the first to know of any updates. In the meantime, stay calm but be prepared.
If you found this useful, please be sure to share with anyone you know who could benefit.
xo Holistic mama doc – Elisa Song, MD
Keep Up to Date on the Latest COVID-19 News:
- WHO: Coronavirus disease (COVID-19) outbreak https://www.who.int/emergencies/diseases/novel-coronavirus-2019
- CDC Coronavirus Disease 2019 page https://www.cdc.gov/coronavirus/2019-ncov/index.html
- WHO COVID-19 Situation Reports: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports
- CDC’s COVD-19 travel advisory page https://www.cdc.gov/coronavirus/2019-ncov/travelers/index.html
References:
- www.who.int/dg/speeches/detail/munich-security-conference
- WHO COVID-19 Situation Reports: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports
- https://www.tandfonline.com/doi/full/10.1080/22221751.2020.1729071
- https://jamanetwork.com/journals/jama/fullarticle/2762028
- https://jamanetwork.com/journals/jama/fullarticle/2761659
- https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30360-3/fulltext
- http://weekly.chinacdc.cn/en/article/id/e53946e2-c6c4-41e9-9a9b-fea8db1a8f51
- https://www.cdc.gov/coronavirus/2019-ncov/hcp/identify-assess-flowchart.html
- https://www.ncbi.nlm.nih.gov/pubmed/31560964
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4032839/
- https://www.ncbi.nlm.nih.gov/pubmed/16789928
- https://www.ncbi.nlm.nih.gov/pubmed/15885816
- https://www.ncbi.nlm.nih.gov/pubmed/16115693
- https://www.ncbi.nlm.nih.gov/pubmed/20934345
- https://www.ncbi.nlm.nih.gov/pubmed/22578462
- https://www.ncbi.nlm.nih.gov/pubmed/18479853
- https://doi.org/10.1016/j.chest.2016.11.036
- https://clinicaltrials.gov/ct2/show/NCT04264533
- https://www.clinicaltherapeutics.com/article/S0149-2918(17)30235-7/fulltext
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4253453/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4253453/
- https://www.ncbi.nlm.nih.gov/pubmed/17609337
- https://www.ncbi.nlm.nih.gov/pubmed/15668926
- https://www.sciencedirect.com/science/article/abs/pii/S1756464619301203
- https://www.ncbi.nlm.nih.gov/pubmed/31377749
- https://www.ncbi.nlm.nih.gov/pubmed/21640201
- https://www.ncbi.nlm.nih.gov/pubmed/24201081
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5921439/
- https://jvi.asm.org/content/81/1/416
- https://journal.restorativemedicine.org/index.php/journal/article/view/46
- https://msphere.asm.org/content/4/5/e00474-19
- https://www.medrxiv.org/content/10.1101/2020.02.18.20021881v
- https://www.nejm.org/doi/full/10.1056/NEJMe2002387
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2778074/
- https://doi.org/10.1093/ajcn/26.11.1180
- https://www.journalofhospitalinfection.com/article/S0195-6701(20)30046-3/fulltext
- https://www.nejm.org/doi/full/10.1056/NEJMc2004973
- https://doi: 10.1542/peds.2020-0702
- https://www.ncbi.nlm.nih.gov/pubmed/32180426
- https://www.ncbi.nlm.nih.gov/pubmed/32182347
- https://www.mediterranee-infection.com/hydroxychloroquine-and-azithromycin-as-a-treatment-of-covid-19/
- https://www.ncbi.nlm.nih.gov/pubmed/21079686)
- https://doi:10.1371/journal.ppat.1001176
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4182877/
- https://pubs.acs.org/doi/abs/10.1021/jf5014633
Thanks so much!!! we appreciate your work and all you do to keep us well informed.
I’m so grateful I can be of help! xo
Thank you!! Very much! Great information. Could this be posted/shared on one’s FB page?
Hi Lotta – we’re looking into how to get FB share button on. In the meantime, you can cut and paste the url to your FB post. Hope that helps!
Is the VClear ok for a 5 yo? And if so, what is the dosing? It doesn’t say on the bottle, but I purchased it after reading your post/article.
Please advise if you can!
Thank you so much for this information and the holistic suggestions to help as they figure this all out!
Yes VClear should be safe for a 5 year old. When my kids were 5, I gave them 1 teaspoon 3x/day when they were sick. Stay well!
Thank you so much as always from one loving mama to another !!
you’re so welcome, Shelley! xo
Thank you for your thorough explanation and wise recommendations. There seems to be a lot of fear circulating because of the unknowns.
Yes, it’s the unknown that scares people. That’s why I wanted to figure out all the facts and share! xo
Thank you for your thorough explanation and wise recommendations. There seems to be a lot of fear circulating because of the unknowns of this virus.
Thank you! I’ll update information as I have it!
You are my voice of reason. Thank you for all you do. Chris 🙂
You’re so welcome! xo
I’m just a Dad but…Wow!…this is great information. So well done and so comprehensive. This goes on the Fridge for handy reference. Thank you!
Might be a little heavy for fridge magnets? 🙂 Thank you so much! I’m so glad you found it helpful!
Just a dad? No no no….you are a * D*A*D * (okay imagine that with rays like the sun bursting out around the word dad)…. you are an amazing parent who took the time, like the rest of us, to avoid the panic stunned public who are like moth to flame entranced by the media, and you have chosen to be calm and seek out the best holistic knowledge from a caring honest medical expert…. you like all the other parents putting their child’s and family’s welfare at the forefront of their action plan, are AMAZING! Thank you Dr. Elisa Song for taking the time to be a cornerstone for those seeking health, and especially in this crisis, and also for everyone who heed’s this very educational and useful action plan. Be well !
Thank you, Joanna, for your amazing and heartfilled comment to Ralph, to me and to all of us.
In gratitude, Elisa xo
Great info. Thanks Dr Song
you’re welcome!
Thank you for taking the time to research, write AND share.
you’re so very welcome!
I think this is a nice summary. My only concern is your recommending bone broth. This whole outbreak started because of animal consumption. And animal as well as animal product consumption cause all sorts of pro-inflammatory conditions in humans.
That is a great point, Erin. I will investigate this. WHO recommends thoroughly cooking all animal products for consumption, and with bone broth, I typically let mine simmer for 12-24+ hours, so I’m guessing this takes care of any possible transmission, which would be much lower anyway in the US from farm-raised animals vs. the animal markets in China. But I could be wrong. I will definitely think about this more and thank you for bringing this to my attention!
A clean, grass fed bone broth powder is my go to!
Thank you for this great research, Elisa!
Hi Bridgit! You’re so welcome! I did the research as much or myself and my kids as for everyone else! 🙂
Thank you!! You have helped ease my anxiety about this. I’ll still prepare, just in case. At what point would you pull the kids from school and homeschool?
You’re welcome! Hmmm… I don’t think I’ll know when I’ll pull the kids from school until I do. But I’ll let you know as soon as the thought crosses my mind!
That’s the best, most helpful article I have read on this topic. There is a lot of confusion going on out there. Did you come across any information on how this virus formed or was formed in the 1st place? Thanks for keeping us sane! Laura
Thank you, Laura! And I have not come across any solid information – I know there’s a lot of speculation but I only wanted to include in my article what I could find accurate references for…
Thank you for the very informative article’
I’m so glad you found it useful!
Dr. Song, that is the most comprehensive article i’ve read so far on the situation. thanks. i shared it on facebook. Angela Lee, Mom and Licensed Acupuncturist
Thank you, mama and practitioner – we need to stick together! 🙂
I posted your article on FB. it is a wealth of information. thank you for bringing it all together.
thank you for sharing!
What about colloidal silver?
I haven’t found any research to solidly support considering colloidal silver with COVID-19, but it can be an effective antiviral. I have used Designs for Health Silvercillin throat spray for the start of any viral upper respiratory infection…
Aloha Dr. Song! As an RN mom, I’m always looking for evidence to back treatments….that’s the scientists in us, right? I’m late in the game to get into these holistic treatments and wondering what kind of evidence there is to back the use of silver as an antiviral? One of my friends swears by it but you’re the first practitioner I’ve heard support it.
Silver has some great antimicrobial properties but I’m not sure that its effect against coronavirus has been studied. I’ll look into it!
WOW, Elisa, this is exhaustive and helpful, indeed! Excellent post. I was in the process of making a similar overview for my audience but instead I am just going to redirect them here. So thank you for doing all the heavy lifting!
The only missing piece I would add to the above regimen chlorine dioxide, which I’ve heard was studied against the SARS corona virus in 2013 or 2014 (I found the paper once, but for some reason, haven’t been able to pull it up on Pubmed since). Apparently one dose of CD kills corona virus dead within 30 minutes. I’ve been traveling for the last 2 weeks in Africa, and drinking 1-2 doses a day of CD myself, just for good measure, and I’m confident about both its potency and safety.
Thank you! And wow – awesome about CD. Can you please send me the reference when you find it and I’ll update the post? 🙂
I’d do some further research on that first
FDA warns against using chlorine dioxide against new virus
By BEATRICE DUPUY January 30, 2020
I’d do some further research on that first
https://apnews.com/afs:Content:8438840420
Amazing, thank you so much!
you’re welcome! 🙂
Thanks so much for all the info. I woke up worrying about this today and your article is a godsend!
so grateful that you found it helpful!
This is amazing!! Thank you so much for all your hard work and time you put into this. I am so grateful. It helps quell some anxiety brewing. What is the brand of mask your kids are wearing?
You’re so welcome! Kenzi and Bodi are wearing the ECO-GEAR Anti-Pollution N95 face mask. But when I just looked on Amazon, it wasn’t available. I’m guessing manufacturers are ramping up mask production and we’ll see more soon…
Thank you for this information! Fight fear with facts – I totally agree with you!!
Yes! Knowledge is power!
Thank you! Thank you! Thank you! Thank you!!! This is very helpful.
I’m so grateful you found the article useful!
Where can I purchase the Sambucus Formosana Nakai?
And thank you for your wonderful study and information
you’re welcome! Unfortunately, this form of sambucus isn’t available anywhere that I can find. I included the study because it was so interesting. I don’t know if sambucus nigra would have similar effects, but in a pinch, it may be one of the best options we have…
This is amazing, thorough, and informative! Thank you!!
you’re so welcome! So glad it’s helpful!
Thank you! Do we need to go through a doctor to get Metagenic products?
Hi Alicia – Metagenics does have to be sold through a practitioner. A local functional medicine practitioner may have it available. Peter and I are working like crazy to get our online store done so people can purchase the supplements I recommend. In the meantime, we have been having people call our office 650-595-5437 and our front desk can help with purchasing these supplements.
I also did some research before I traveled and found that Licorice Root Extract and “griffthsin” in Red Algae kill the glycoprotein outer shell of the corona virus and then the virus can’t replicate. Did you see you this info in your research. This was published by GreenMed from the Journal of Plant Medicines by Case Abrams PhD. https://plantmedicines.org/plant-medicines-fight-wuhan-coronavirus/
Thank you so much! I love finding new resources. I will definitely take a look at this!
With the GreenMedInfo, additional help is here too …
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4058675
This really helps to ensure Case Abrams’ insight to what does work.
Thank you so much for all the information. I can’t find that type of elderberry anywhere? Only the black elderberry. Also, what do you think of monolaurin and cat’s claw as ways to prevent the virus from getting too serious?
Unfortunately the Sambucus Formosana Nakai is not available commercially as far as I can tell. Since we don’t know much about what will work specifically against 2019-nCoV, I think that having other natural antivirals that work for different viral illnesses is a better option than nothing. I have used both monolaurin and cat’s claw effectively for patients with other viral illnesses for sure!
I see someone above mentioned chlorine dioxide? Does the average person need this? Sounds toxic?
Dr. Song, you’ve provided very good fact based information about a virus that still has little facts. I’d like to mention two points.
1. Regarding the guidance about wearing masks. I’m pleased that you are writing in support of masks as many clinicians and administrators are still making claims based on “research” that masks are not effective. One of the points I try and make to people is that while the mask might not be sealed perfectly, nor be able to filter particulate as small as a viruses, they serve an additional benefit that is equally as important. They keep people from putting their hands near their face and nose, which most PH providers agree is very important to stop transmission.
2. One issue you didn’t point out and I think is important to explain, is the data on re-infection or people not being fully recovered and testing positive again. Either we have a virus that is unique in it’s ability to reinfect quickly with little to no immunity, or are we dealing with a respiratory HIV type virus that transmits airborne and might not cleared like the traditional flu virus.
I agree with your position to limit air travel and further suggest people limit close proximity contact with others.
Further, I sincerely hope the CDC changes the guideline for testing immediately to include anyone with flu symptoms and negative for flu. I hope clinicians apply pressure to their state PH depts. to apply pressure to the CDC as you know this virus is not being tested for community transmission.
All the best
thank you for your thoughtful reply!
thank you for your thoughtful comments – I appreciate it!
Good job Doc. From a functional immunologist, you did a solid job here. I’ll be sharing this article
Thank you so much!
Well done. Thank you for your research and common sense approach. It’s a breath of fresh air. 🙂
Thank You Elisa for doing the research and you sharing it with all of us.
Great info, thank you. I’m also wondering if I’m unlucky enough to contact this virus, wil I be immune from contracting it in the future?
I don’t anyone knows yet what future immunity will be like. We’ll have to see what happens…
What about taking silver? I saw on the Jim Bakker Show that silver would kill the Coronavirus
I haven’t seen any research on silver and coronavirus. It may be helpful, but I only wanted to provide information that I could back up with evidence. If you have any references, please do share!
I greatly appreciate this information. It has eased my mind a little. All of this is so so helpful.
I’m so grateful that I can help spread some calm among all the fear…
This is truly an eye opener I am glad to know
the truth. Thank you for letting it be known what we
can take to keep our children healthy and protected.
I will be doing the nose rinse as well as my husband
and grandchildren.
Thank you, Barbara So glad you found the article helpful!
What are your thoughts on inhalers? I have Alvesco and levabutoerol (both given in case of asthma) — would you recommend using those if coughing gets severe if any of us get infected by this virus?
If you’re wheezing, I would absolutely use inhalers as recommended by your physician. And if cough gets severe or wheezing develops, please do see out medical advice from your physician. Best of luck!
Hi Elisa! Just read this via another friend’s post on FB. Will follow you. We moved to SoCal a few years ago. Keep up the voice of reason!
Thank you! I so appreciate your comment!
I just flew from Ontario ca to Sacramento ca and back Monday and Wednesday and have been panicking because of the unknown and if I got it. I followed proper hygiene methods as I’m a germ freak. This helped my anxiety and panic attacks I have been having. This is the only flight I have had to take since January and again until April or later. Thank you for the information.
you’re so welcome! That’s what I was hoping this article would do – help people feel more calm. But fear and anxiety will only serve to weaken our immune systems. Stay healthy! xo
Thank you for this information!!
you’re welcome!
Thanks for your informative information.
you’re so welcome!
This is the best, hands down, explanation I’ve read on what we can do (not just our kids) that is practical, natural, with science to back it. Thank you for posting! Glad that I found your site!
Thank you so much! That’s exactly what I was hoping this article would be!
I appreciate all your research and I was very excited about
Sambucus Formosana Nakai, however, I cannot find this anywhere- only pictures of the plant. Not available as a supplement it appears. How do you propose we consume this???
Unfortunately, I don’t think this form of sambucus is available commercially. I wanted to include the research in case it sparks some studies, and perhaps a look at if sambucus nigra (black elderberry) may be useful…
Thank you so much Dr. Song! Iʻm happy to see what our family has been doing to strengthen our immunity is in line with your recommendations here.
I was able to get a kids cloth mask for my child that I will be flying with soon (an essential flight), mainly for the purpose of helping to keep her from touching her face. Can you share how you’d wash/disinfect your kids’ non-disposable masks for safe reuse?
So glad you’re already implementing these immune-boosting measures! As for the cloth reusable mask, I would definitely follow the manufacturer guidelines on how to best care for it. Safe travels!
Best Practical Information I Have Seen Out There – Keep Up The Good Work! You Are The Best…
thank you, Dr. Hopkins! You are the best! 🙂
Thank you so much for this timely and incredibly valuable wealth of information. You are a wonderful human being and physician. Also grateful!
Thank you so much!
Thank for doing all this work!
good info…i think the infected person i Solano county is a she not a he as you mentioned…but overall thanks for the info
you’re right! thank you – just updated the article.
Wow! I want to say thank you so much for this article!!! I have been so concerned with this virus and the potential continuation of spreading especially with a 10-MO and this has been the best article I have found. I appreciate you taking the time to help us all and I will continue to share!
Thank you so much! I’m so glad it’s helpful!
Thank you for taking the time to share this valuable and informative information. Thank you for also providing credible sources. I appreciate you!
Especially in this time when we don’t know what to trust, I tried to only put information that could be backed up by evidence. So glad you found it helpful!
Thank you for sharing this information and helping me make informed decisions for my family. I appreciate you!
Knowledge is definitely power. So glad this helped!
Wow. Thank you for this information!!!! My parents live abroad in Europe so we’ve discussed it but we also don’t have TV service so the media info we have gotten is very limited (thankfully). I SO appreciate having reliable information to share with others as well.
Low media info may be one of the best things to reduce stress during this time! So glad you found the information useful!
Dr. Hopkins,
Thank you so very much for all of this information!
I’m sure many people like me that have read this, are less stressed about what we can do to prevent getting this awful thing that has come into the U.S.
I pray for my family and yours and all of the U.S. citizens that must travel. My daughter and husband are flying to England in April for the Marathon and then on to Paris for a few days of sightseeing and fun I pray for their safe travels but also scared for them!
Looking forward to more information on how to survive this thing and to be able to safely travel!!!
Thank you again for this information!
Hi Judy! It’s Dr. Song. So glad you found the article helpful. Not sure which Dr. Hopkins you meant?
thank you
Well done Dr. Song! I so appreciate all the time and effort you put into researching and writing this so we all feel calmer and factually informed. Your the best!
Thanks so much, Christina! You’re the best! And one of the reasons I researched and wrote this article! xo
Thank you, Dr. Song!
you’re so welcome!
Dr Song,
You are amazing! I’m so grateful that you are my doc! Thanks for sharing this information and doing such thorough research.
Thanks so much, Sarah! So glad it’s helpful!
Thank you for this very informative article. I do agree that everyone fears the unknown. So glad I read your article to shed some light on what I didn’t know. Thank you!
Awesome article. Thanks so much for empowering moms and dads far and wide!
Thanks you so much for the exhaustive research! This is the most sane and comprehensive information yet! I’m particularly interested in the bacillus sp strain LBP32 strain you mentioned. Do you know what supplement manufacturer/brand has that or includes it in their formula? Thank you!
Unfortunately, I don’t know if a supplement that currently carries this strain – I wanted to include all the relevant research in hopes that scientists will take notice and expand their research efforts to potential natural therapies…
I went to 5 stores today looking for this strain, to no avail. And now I’m just seeing the response to your question. Darn! I was really hoping to get my hands on some of this to send to my son who lives in France.
Hi Maryanne – unfortunately this strain is not available commercially that I can find. I included it for research purposes. I do not know if other strains would have similar benefit but we do know that so many probiotics strains have amazing immune supporting properties in general…
Thanks for your reply! I’ll do some research on other types of probiotics. I know there are many good ones out there. 🙂
Awesome info from an awesome doc! Thank you so much for your valuable insight.
Thank you so much, Andrea! 🙂
Read every word and every comment I’m so grateful for this amazing guide and reference what tremendous effort on your part WOWZAAA I am so very grateful. Will be enforcing nasal washing more but I have a nail biter kid so the anxiety about hand-washing is intense. We do vitamin D3 with k for optimal absorption 5 to 10Kevery other day, Sovereign Silver and Garden of Life Raw Probiotics do u think its varied strains are potent enough? Saw you on friends pg and will be sharing on mine!! So happy to have found you but this piece is WOWW!
Yes it was a tremendous amount of work but I’m so grateful that it could help my family, families in my practice, and families around he world! I think the Garden of Life probiotics are very good, and it can be helpful to rotate probiotics as well!
Great article!
Indian Authorities Propose Use of Homeopathy to Prevent Coronavirus | The Scientist Magazine®
https://www.the-scientist.com/news-opinion/indian-authorities-propose-use-of-homeopathy-to-prevent-coronavirus-67075
You lost all credibility when you couldn’t even properly use the word “everyday.”
Thank you for your useful comment. I’ve updated the blog.
Heaping coals. Well-played, Doc. Much love!
Not sure what “heaping coals” means? Glad you found the article helpful! 🙂
You are a class act, Dr.Song!
Thank you!
Thank you Dr. Song for this helpful information. I appreciate all of the work that went into your article and it covers so many areas. Now that Nebraska has its first case, my stress level kicked up quite a few notches, but knowing that stress is not helping my immune system, I’ll try to reel it back in.
I’m also happy that you addressed nasal irrigation — something I recently started doing at the suggestion of my ENT. He also mentioned that doing so could remove viruses from that area before they have a chance to take hold. Once I got past the waterboarding feeling from it, I’ve learned to love it and look forward to it twice a day.
Thank you very much for this informative and helpful article, Dr. Hopkins.
I found this really helpful, informative and up to date. I was also impressed by the evidence-based data on natural remedies. It is important not to neglect these, especially as there doesn’t appear to be anything useful in ‘traditional’ medicine. As you point out, they are likely to be much more affordable than any new antiviral agents or vaccines which may become available. I hope you will be able to update us as appropriate.
Bill McWhirter MD
Paediatrician
Hi Dr. McWhirter – so grateful that other MDs find my article useful! And yes – I will be updating as I get any more useful information!
Thank you Dr. Song,
I am so glad to see this article and finally find reliable information and tips for a preventive holistic approach in the midst of the current hysterical climate, this is really helpful.
So glad you found it helpful!
Thank you so much for all work you have done to help us be more informed from a professional level. Thais has helped me so much and I feel more at ease. The virus is yet to hit Australia on a large scale but it’s good to be prepared for it if and when it does.
You’re so welcome. Yes – being prepared calmly is the best way to go!
If I get corona, then get better, will I get it again? Immunity?
It’s hard to say – 2019-nCoV has already mutated, so yes, you could theoretically contract both of these strains. And coronaviruses in general mutate quickly, which is why people get colds over and over and don’t build immunity. Thankfully, this second strain appears to have milder symptoms associated with it…
Dr. Song, thank you SO much. I’m confused by the “nasal irrigation” concept. With a neti pot, I’m literally irrigating and washing out my nasal passages, with salt water running out into the sink. With any nasal spray, I inhale, my nasal passages water, and then I end up swallowing or having the liquid run down the back of my throat. It seems that with coronavirus, I’d end up swallowing a lot of viruse particles that might be washed out of my nasal passages. Am I doing this wrong, and maybe I should make a better effort at blowing my nose after the spray? Help! I’m probably doing it wrong. Thank you again for this very comprehensive list!!
Such a good question, Beth! If you end up swallowing some saline, your stomach acid should kill most of the microbes in it. But yes, please do then lean forward as you’re spraying and then blow your nose after a minute or so!
Thank you for this reassuring and empowering research article! I am happy to find that many remedies I have can be useful now. I also want to add–I have not gotten the flu in many years, even with others around me having it, since I stopped eating wheat, corn, and dairy products. My cat advised me to stop eating all wheat, corn, and dairy, because they are treated with toxins. So I did. Mostly. Occasionally I return to eating some, and then I feel achey and sick. I also have foudn that if I eat a lot of salt, I get a cold–even a significant cold, for a week or more. A bag of chips, or crackers, or salty chicken,… it makes me get a cold. So, my health has been super strong when I avoid salt, wheat, corn, and dairy! I am outside walking my dogs for an hour to two hours per day. I assume this brings me plenty of Vitamen D. Thank you!
A clean, healthy diet is one of the best ways to stay healthy! So glad you’ve found what works for you!
I am so grateful to you for compiling this report. Stay well and many blessings to you and your family. Thank you, thank you.
Thank you so much for the information. I am sharing this to my FB and forwarding this to my son who is in Incheon South Korea right now.
Reading this made me calm and be more positive. He is an English teacher and will be moving to Japan in three weeks.
Thank you very much! And bless you Dr. Elisa Song!
Best wishes to your son during this stressful time! I hope he stays healthy and well…
Thank you so much for this article, Dr. Song! I just posted it on my facebook page after spending the past few days talking about it and sharing it individually with various friends and community members. I was saying very similar things before reading your article to everyone I knew, but, until there was a written and researched article such as this, it was difficult for the people I was speaking with to feel reassured or comforted. I am not a doctor (yet) but am in school currently to become a Naturopathic Physician; I also grew up in a medical family. I recognized the disconnect that was happening nationally between various articles and headlines and the actual reality of the nature of this newer virus, and the fact that people were not reading primary sources but only going by various things they had heard in passing, or running with alarming headlines without doing further research. When I am officially a doctor (and still now, before) I hope to be an educator that brings a calming and grounding voice of reason like yourself. So, thank you again, I have shared your article with many people that were feeling panic, and they are now feeling reassured and are sharing it with their loved ones.
Thank you so much, Rachel! You will be an amazing healer and educator. Good luck in all of your endeavors!
Thank you SO MUCH for doing all this research! I love when Doctors care enough to share without charging! YOU are truly someone I can trust and I will share all your information with the elementary school I work at and the one my grandchildren attend. God bless you! Looking forward to any and all updates! Stay safe❤
thank you so much! I so appreciate your taking the time to comment! xo
Hi, great article! Thankyou. Very thorough and informative. Is it possible to get a link to the study referred to regarding hand washing even without soap being superior to alcohol based hand rubs please. I believe this to be true and would love to have the evidence to back it up thanks. It says reference 36 but your list only goes to 32.
Thankyou and have signed up to your newsletter, looking forward to more of what you have to say. Best wishes to you and your family. Christine.
Here’s the link: https://msphere.asm.org/content/4/5/e00474-19! And I’m just about to publish an article on how to really wash your hands! 🙂
Wow, THANK YOU. I’ve been following COVID-19 developments via the New York Times (and I’m in Australia) but THIS is so far the best, most informative, fact-filled article I have seen. Such gratitude to you for taking the time to thoroughly research the facts and share them with the world.
you’re so welcome!
Very informative! Thank you!
Great information; very helpful. thank you.
Thank you so much Dr Song! We truly appreciate your efforts 🙂
There appears to be a significantly mistaken statement regarding “Wash Hands Frequently” (assigned Reference #36 but not included in ref. list): “…This study found that washing hands even with plain running water without soap was more effective than ethanol-based hand disinfectants at killing the Influenza A virus! (36)”
Is this a typographical or uninformed error? Common sense tells us it is not a credible statement.
Hi there – here’s the link to the handwashing article. The investigators studied an alcohol based disinfectant with plain running water. It’s a small study and needs to have larger numbers, but is fascinating: https://msphere.asm.org/content/4/5/e00474-19.
Hmm, I don’t think that this study was comparing alcohol with plain running water. The study compared alcohol based with “antiseptic hand washing.” They never actually defined antispectic hand washing, but linked a video from the New England Journal of Medicine. This video is on youtube: https://www.youtube.com/watch?v=uGmMDC-4IMY
In this video, antisepectic hand washing is with soap: https://youtu.be/uGmMDC-4IMY?t=387
I agree the study is actually very confusing. But if you scroll to the end of the paper, you will see that the researchers did use plain running water. I will definitely check out the videos, though. Thanks!
Found it, thank you! “Regarding the AHW regimens in this study, handwashing was practiced using running water only, without using plain or antiseptic soap.” I
For the record, WHO seems to define AHR as with soap, but that’s an error by the authors/reviewers/editor, not by you. Thanks again! https://www.ncbi.nlm.nih.gov/books/NBK144046/
Thanks from your ex-CA and now in Ireland patients! Ireland just got its first case this weekend and I knew I would be checking for your gems of knowledge! Elaine
stay well, Elaine!
Hi Elaine, i am also in Ireland. I work intuitively with herbs although i have a pharmacy degree, nutritional diploma and functional medicine training. I dont know if it is science enough for you; but i always tap into what herbs may be of use in meditation and then get to the research after. the following showed up as helpful to us here in ireland and i am sure, if you were concerned a herbalist can assist. Sambucus nigra (despite the above. it is one of Ireland yearly anti-viral remedies and i do believe mother nature provides… so why not, at worst it will not help. at best it will), rosa canina (rose hips), olea europea (olive leaf extract), echinacea angustifolia (not purpurea), scutellaria baicalensis, and interestingly nettles and cleavers which are popping up now and make great pesto. many reasons both from an anti-viral and an immune perspective and more to include these as a strategy. i was shown that scutellaria is more a treatment than a prevention. and i do believe that there is research on this and even a patent on its anti-viral effects from one of its constituents. hope this helps.
Thanks for gathering this information. A report I just heard on those in Japan who wear masks mentioned that they seem to take them off in bars and restaurants so I wonder why I put them on in the first place. And especially wear them on the streets with fresh air and take them off in a building with recirculating air. A mystery to me.
It seems to me that modulating and strengthening the immune system would be most helpful. There are products available with AIE10 in them. Our family members have taken them for a long time and will surely continue now. And… Wash our hands
Yes, most people do not wear masks the right way, and don’t wear the right masks… Keeping our immune systems strong will be one of our best defenses.
This article is so helpful and approachable–thank you so much! Which Vitamin D3 do you recommend and use for yourself and your kids?
Thank you! We use Vitamin D3 drops by Orthomolecular Products, but there are many good brands easily available like Nordic Naturals…
Thank you so much for your response. I’ll look into the Nordic Naturals gummies for the kids. What do you think about the Designs for Health Vitamin D Supreme for adults?
I work as a nurse in long term care, this has been very helpful. Many thanks
you’re so welcome!
Thank you so much for this amazing information! I have a 9 yo daughter with viral induced asthma – would that be considered one of the pre-existing conditions for higher risk? Just trying to see if there’s anything more I can do to protect her. Thank you!
Hi Ujwala – it’s hard to say. Asthma is an increased risk factor for influenza complications in children, but we don’t know yet if it is for COVID-19 in children. I do believe the best way to protect our kids is to support their immune systems as I outlined above. Best wishes to you and your daughter!
Greetings, I’m very grateful for you Consolidating all of this information.
so glad you found it helpful
Thank you Doctor for a very comprehensive and holistic post – as always!
For kids and adults who are immune compromised or with susceptibility to auto-immune condition, do the suggestions apply equally well. As you noted, they may not hv fever due to poor immune condition. Are there other symptoms to watch out for.
Most schools seem to be deep cleaning, which could potentially result in overload or exposure to strong cleaning chemicals from the environment. Do you recommend keeping such kids off school to keep them safe for few days/weeks.
Thanks,
Sankar
Hi Sankar – that’s a great question. It still seems that children, even with underlying chronic conditions, seem to be relatively spared. So I think that going to school is probably fine unless the school shuts down due to exposure. And for cleaning chemicals, I think these should be ok with a good detox regimen in place and wouldn’t be cause to miss days of school… Take care!
Wow, that was super informative and all the information we need to arm ourselves against this virus. Thank you so much for the information-packed article!!
That’s exactly what I wanted it to be! So grateful for your feedback!
Stick To The Facts: “The Transmission of COVID-19 Coronavirus” (The Sad Reality) >>
I think it is important to start any discussion about the “Coronavirus” with a little perspective…and some factual reality-based therapy…
FACT: Each year in Australia, influenza kills on average 3,500 people.
FACT: The best predictor of who is susceptible is age – 3,000 of these deaths are people aged over 50.
FACT: Death rates for influenza in Australia are below 0.2% of people who contract the disease.
FACT: Estimates suggest close to half a million people die each year from influenza worldwide.
FACT: The last global pandemic – the ‘H1N1’ (also known as the ‘swine flu’) – resulted in around 19,000 hospitalisations and about 200 deaths in Australia.
FACT: It is estimated that one in five people worldwide contracted swine flu and the death rate was 0.02% (even less in Australia).
FACT: Coronavirus (properly known as COVID-19 or SARS-CoV-2) has so far resulted in 1 death (thus far) in Australia and around 20 people hospitalised.
FACT: Reports indicate COVID-19 is more deadly than influenza – early estimates suggest death rates from COVID-19 are close to 1%.
FACT: This may change over time as it is likely that many people with COVID-19 only experience mild symptoms not requiring any medical intervention and are therefore not counted in the statistics.
FACT: Many experts believe it is now inevitable that COVID-19 will continue to increase in prevalence. Although many of us may eventually contract COVID-19, most of us will experience relatively minor symptoms.
FACT: As with influenza, the most susceptible to COVID-19 are the elderly.
SPECULATION: These alarming statistics about influenza (a death rate higher than our road toll) are exactly the reason governments and health experts are so concerned about COVID-19.
REALITY: No-one wants a disease equivalent to influenza spreading widely in our communities, even if most of us will only experience mild symptoms.
REALITY: Clearly, preventative measures are warranted and the likely increase in the disease will place increased pressure on our health services, so we need our health system to be prepared as best it can.
SPECULATION: The cumulative impact of bushfires and COVID-19 means an already brittle economy is now facing the very real possibility of a recession – two quarters in a row with negative GDP growth.
SPECULATION: The loss of economic activity (tourism, international trade, etc.) will translate into a loss of government revenue at exactly the time when governments need to stimulate investment & job creation to maintain growth.
SADLY, OUR REACTION: People, this does not mean everyone stocking up on toilet paper! Crazy, hey???
Love this article thank you!
Can you purchase Sambucus Formosana Nakai anywhere???
I’m so glad you found this article helpful! Unfortunately, the Sambucus Formosana Nakai is not available commercially as far as I can find. I included it here for research purposes, but even though there’s not evidence for Sambucus nigra against coronavirus, there may be some crossover. Stay well!
Thank you for this great piece which manages to be both an effective distillation of hard data and a primer on what we can do to mitigate our risk of exposure.
I also wanted to pass on a link to 2014 report by the NCBI regarding a study focused on the efficacy of Sambucus nigra on another coronavirus, namely IBV. Please see ==>https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3899428/
thank you so much! I will include this in the post!
Thank you! My kids are grown but I nanny a little 3 year old so this is very helpful. I ordered Metagenics Ultra Flora Balance for myself and my husband. Should I take one or two per day? Also, were you a Peds Resident at UCSF? I recognize your name as I am a retired Pedi RN and worked there from 1994-2010.
Hi! That was definitely me – I was a UCSF peds resident from 1997-2000! Small world! For adults, the recommended dosage of Metagenics Ultra Flora Balance is 1 cap 2x/day. Stay well!
Wow this is the best info I’ve read yet and I’m a Nurse in a mess of information… thank u so very much for all this excellent info and thoughtful research
you’re so welcome!
I’m glad to hear about the low number of deaths in South Korea, but I don’t think you can use those figures to calculate the mortality rate. Among the 6,088 who have been tested are more people who will end up dying from the disease. Knowing the final number of deaths from among the 6,088 tests, which we’d have to wait a few weeks for, would give us the mortality rate.
So, I’m thinking we should let the epidemiologists calculate the mortality rate. But I really appreciated the rest of your info.die
You’re absolutely right that we don’t know yet the full extent of the death rate in South Korea. But at least through their experience we’ll get more accurate data. The key is to start testing and test widely, which unfortunately, for us in the US, we are way behind the eight ball.
I think the mortality rate in South Korea might be one of the most accurate, given their approach to aggressively testing as many people as possible, an approach that the rest of the world could learn a lot from!
Thank you so much, Dr. Song! I’m a Naturopathic Physician and this aligns with our philosophy. I have shared your article on FB and it has gotten multiple shares.
Thank you so much for sharing, Dr. Stubbe! So grateful you found it helpful!
Good afternoon Dr. Elisa. I’m not quite sure if this is going to be a redundant post or not, as I did it submit a comment a few days ago, but I haven’t seen a response yet. Please forgive me if you’ve already responded. I am a mother to five children, my youngest is 11 weeks old and was born at 35 1/2 weeks. We are due to travel to Seattle next month and then onward to New Jersey. I realize that this virus has been shown to affect only the immunocompromised and the elderly, most severely, however, would it be prudent of me to have our children where the N 95 mask during travel to protect the immune system of the baby? Or is it quite useless? We are a pretty germaphobic family in general, so handwashing and hand sanitizing are already high priorities for us. We always wipe down all surfaces on the airplane as well as anything purchased in the airports, and washing hands or sanitizing after touching any surface at all. I do high doses of vitamin C ascorbic acid for all of our children, as well as elderberry, probiotics, Immune support echinacea powder, and colostrum tablets. My newborn is exclusively breast-fed. Any advice you can offer me regarding this travel would be helpful. If traveling with this young of a baby through those compromised areas is too risky, I would appreciate hearing that. Thank you in advance for all of your help. This is a wonderful article and I have shared it countless times with several avenues I am connected to.
Hi Kristin – I know many people will be wearing masks while traveling, and if you’re taking an abundance of precaution to boost your immune system and wipe down all surfaces, I don’t think it’s unreasonable to wear N95 masks, and hopefully they will fit your children adequately. In that very small study of Chinese infants, even very young infants seem to do fine, but if she were my baby, I would wear her in a carrier and keep her head covered while she’s sleeping. Since we are seeing different numbers and learning more everyday, next month is a long time away to know what the extent of the infection risks are with air travel, but I will keep my fingers crossed for your family to have a safe and healthy flight! You’re doing all you can! xo
Thank you so very much for taking time to reply. I appreciate it. I failed to mention that I babywear her most of the day and plan to do so through the entirety of the flight. Thank you so very much for the reassurance and helpful advice! I appreciate it!!
Dr. Song, I’m one of your followers. You bring a package of calm during the storm. Although children seem to be less affected than other target populations, my 9-year-old is asthmatic so we are particularly and especially concerned. We are getting so many mixed messages from the various government offices that it’s been hard to figure out which path to take. Given that he’s part of the vulnerable population and his family still has to be on crowded public transportation on a daily basis – it’s hard to hear our governor continue to say that children are relatively ok in this… and it’s even harder NOT to hear how to build your immune system while wading through the germs. So grateful for you. I actually turned to you when this first hit and so glad to see you came through for all the people that need you and your voice during this difficult time.
-Regina
Hi Regina – I can’t tell you how much your comment means to me. I’m not going to lie – it takes a ton of time away from the kids to keep writing articles so that parents can be armed with the knowledge that I really want them to have, and your comment makes all the effort worthwhile! xo
Thank you so much! All of the information and facts presented are so helpful to have!
Thank you so much for such a reasonable, calm and well-researched post, Dr. Song. For those of us with children or teens with autoimmune disease, would you consider it appropriate to start limiting social activities, or is that an overreaction at this stage of the epidemic?
Such a great but difficult question to answer. I think that if your or your child’s autoimmune disease is under good control and you’re optimizing health with an antioxidant-rich diet and immune-supporting lifestyle, it’s likely fine to continue regular activities. But we just don’t now… So I would make sure your kids are washing hands frequently and getting all the immune supports they can. Stay well!
you’re such a gift to so many! thank you.
Thank you so very much. This is such a great article and really put my mind at rest.
I’m so glad I could help with more calm in this time of panic.xo
Your article is an excellent collection of information, and I am grateful to you for putting together such a useful resource! I hope that it will help many people to more effectively address the challenges facing us with COVID-19.
Re. NASAL IRRIGATION: It might be helpful to note that nasal irrigation can create unexpected health risks if someone uses liquids other than those ones specifically recommended (distilled, sterile, or boiled, etc.), or does not sufficiently clean the entire container and rinse it with recommended liquid.
https://www.webmd.com/allergies/news/20120912/sinus-infections-nasal-washing#1
Sinus Infections Linked to Nasal Washing
Using Tap Water in Neti Pots and Other Devices Tied to Tough-to-Treat Chronic Sinus Infections
However, if appropriate measures are used, it seems like nasal irrigation may be very helpful! Thank you for sharing about this less-known health treatment!
Thank you for your thoughtful reply! Yes, as always, we have to do things in a safe and clean way!
I’m worried that my daughter might catch the COVID-19 disease. Thanks for these tips from the pediatricians. I shall then follow your advice to wash my hands frequently and get ourselves checked in case my daughter gets one.
stay well!
Thanks Elisa – so comprehensive and calm! Appreciate this and the hand-washing blog and making a 60% Alcohol-Based Hand Sanitizer. Sharing all three as links on my blog
I recently learned about Lomatium so I’m pleased to see it mentioned here.
Curious about your thoughts about social isolation, not traveling, no attending big events etc in order to slow down the spread in the USA, Australia and other countries now that we know more about what is happening in Italy in terms of them being overwhelmed with there not being enough ICU beds and ventilators?
Hi Trudy – as we head into Spring Break in the US, this is the million dollar question… I am personally limiting all nonessential trips to stores and travel plans. Given that there are likely many untested asymptomatic and mildly symptomatic people in our communities, I don’t want people to be paranoid about going out at all, but be aware that in the next coming weeks, exposure is likely going to be the norm, and maintaining social distancing will be an important way to slow down spread…
Dr Song,
Can you please provide research for your “common sense” recommendations? I have never heard of nasal irrigation being an effective measure for prevention of respiratory illness. In fact, I worry that irrigating the nasal passages may remove part of the mucosal barrier that the body uses as its own protection against viral illness. You may be actually making it easier for pathogens to enter the body by removing the IgA antibodies present in the mucosa. I am disappointed that you use research in the beginning of the article to lead people to believe your information is evidence based, but then you stop providing evidence when it comes to making “common sense” recommendations. This gives people a false sense of security against protecting themselves from illness and could actually lead to harm.
thank you for your comment. I will update the post with link to research showing that:
“One RCT of 60 adults evaluated spray SNI as preventive therapy for viral URI. In this study, those receiving a preventive daily spray SNI reported significantly fewer episodes of URIs, shorter symptom duration and fewer days with nasal symptoms compared to those without a preventive SNI care.”
The link to the full-text article is here: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2778074/
“department before seeking care. Contacting them in advance will make sue that people can get the care they need without putting others at risk.”
Might want to correct the typo for sure / love this post thank you for taking the time to put it out there!!
oops – thanks SO much for pointing that out! It’s funny how you can proofread something a gazillion times and still miss things!
Wow @ the time and effort that went into this article! So impressive…thank you so much!!! And also thank you for allowing us to share with others
you’re so welcome!
I have followed you sporadically for quite a while, and always appreciated the clear, well-based information you offer so freely. But this is FAR above and beyond. Bless you for the sacrifice of time and energy necessary to put together this timely and incredibly comprehensive guide for navigating COVID-19. And you’re responding to the comments as well! Amazing! You are a gift. Please let your family know that we are grateful to them for supporting your efforts to be available to all of us in this way.
Thank you so much for your kind words. Kenzi and Bodi know that I’m doing this research as much for them as for all the other kids and parents out there to keep everyone as healthy and calm as possible. I am grateful to be able to share this information with you, and to have a family that supports me in doing so. xo
I agree with most of the data. We have to be careful not to forget we are also in the middle of the Influenza season. Many people are giving up on elderberry because of the possibility of an immune over-reaction (Cytokine Storm), this is a very unlikely for a healthy person. If a person has symptoms of a virus I recommend that they get tested quickly to determine if it is the COVID19 or regular Influenza or a different Coronavirus. As you know if a person is having an increased fever and possibility of a Cytokine storm simple blood tests can be performed (serum Ferritin, & CRP) to see if they and their doctor need to be concerned.
thank you, Dr. Petro! Unfortunately, ability to test for COVID-19 in clinician’s office is still severely limited, which is so frustrating. But yes, other respiratory viruses like influenza should absolutely be ruled out as well.
Hello!
GREAT information here. Thank you so much. I just tried ordering the Metagenics supplements you recommended, however, the site prompts for a practitioner code. Are you able to provide that or do you have other recommendations?
Hi Jennier – we don’t have a code, but for people who would like to order, we are having them call our office at 650-595-5437 and our front desk can help you. Take good care!
I greatly appreciate all of the info you have passed on to us!!! I spent 5 weeks (starting 5th of Jan) in my home by myself with some sort of flu, etc. Not much fever but congestion and coughing up mucous from my lungs. I’m not sure what it was, but I mostly did some natural things to fight it. These suggestions from you will be very helpful if I get sick again. I’m 78 yrs old and live alone–my husband passed away last Sept. One of my daughters has learned a lot about natural cures and she lives in WA state and I am in UT but she coached me thru it. I am hypoglycemic and do eat a lot of veggies and fruits and avoid sugar, carbs and processed food. This info is very much appreciated. I’m not computer savvy however.
So glad you recovered and have a lifestyle that supports your health. Stay well!
Thank you for researching and compiling all this information! 🙂
you’re so welcome!
Thanks for this article. So much helpful information.
WHO is now saying that neti pots and nasal sprays can cause coronavirus infection because they “push” the virus from the nasal passages into the throat and lungs.
Your article recommends neti pots and nasal sprays.
What do you recommend now with WHO’s stance? Sometimes they are out of date…
Hi Liz – thank you! Can you please point me to the WHO recommendation against nasal irrigation? I will of course change my recommendation if there is any evidence that it can increase risk of coronavirus infection, but the studies I’ve seen show benefit against protection from upper respiratory infections. I always am grateful for people sending me the latest research that I may not have seen! xo
It’s on the WHO website plus CNN carries an article as well specifically saying not to use neti pots or nasal spray with COVID-19 as they can push the virus from the nasal passages into the throat and lungs.
This is specific to COVID-19 so the research you mentioned does not apply.
Your comment intrigued me, as I’ve started using a neti pot. However, I can’t find the reference. Please look through your browser history and post the link
Here’s how I tried to find the reference:
Here’s a google search for pages posted in the last month with “neti pot” OR “nasal irrigation” on who.int, i.e. the WHO’s website
Your search – site:who.int (“neti pot” OR “nasal irrigation”) – did not match any documents.
https://www.google.com/search?biw=1281&bih=729&tbs=qdr%3Am&sxsrf=ALeKk00t2W57v4xeKRvcVV2i11K_nHuYBA%3A1584421102110&ei=7lhwXpyYBpbn-gT8irGYBA&q=site%3Awho.int+%28%22neti+pot%22+OR+%22nasal+irrigation%22%29&oq=site%3Awho.int+%28%22neti+pot%22+OR+%22nasal+irrigation%22%29&gs_l=psy-ab.3…84069.87200..87570…0.0..0.88.1325.19……0….1..gws-wiz._RbkqGSjlq4&ved=0ahUKEwicx9zH3KDoAhWWs54KHXxFDEMQ4dUDCAs&uact=5
Are here’s the same on CNN.com
Your search – site:cnn.com (“neti pot” OR “nasal irrigation”) – did not match any documents.
https://www.google.com/search?biw=1281&bih=729&tbs=qdr%3Am&sxsrf=ALeKk02E-mPS0_5zSJDCmu73KHTgbC9cGg%3A1584420879648&ei=D1hwXteQJ8Lj-gSGlYXYAQ&q=site%3Acnn.com+%28%22neti+pot%22+OR+%22nasal+irrigation%22%29&oq=site%3Acnn.com+%28%22neti+pot%22+OR+%22nasal+irrigation%22%29&gs_l=psy-ab.3…211751.220787..221848…2.0..0.84.1969.28……0….1..gws-wiz.44CzMTIubbk&ved=0ahUKEwiX1NLd26DoAhXCsZ4KHYZKARsQ4dUDCAs&uact=5
@Liz Sutherland your comment is really intriguing, but I can’t find anything posted about “nasal irrigation” or “neti pot” on http://www.who.int in the last month, let alone a connection to corona virus.
Your search – site:who.int (“neti pot” OR “nasal irrigation”) – did not match any documents.
Please review your browser history and share the link
Thanks, along with everyone else for your information, and even more, your responses to posts here – something most others don’t bother to do.
Since stress is such a factor in immunity, I recommend taking a look at Nick Ortner’s EFT tapping videos on his Facebook page, The Tapping Solution Community, https://www.facebook.com/groups/539801006221362/ I expect there other resources for this but it worked for me!
thank you so much for sharing! Nick Ortner and tapping is an amazing resource to support a healthy stress response during this time!
Thank you for the post. This has eased a lot of my anxiety. My biggest problem, however, is that suggesting people wear n95 masks (at any time) takes them off the market for healthcare providers. I am a pregnant ICU nurse will be in frequent and direct contact with patients testing positive and critically ill. We have had only 2 confirmed cases in my hospital so far but are already seeing critically short supply of masks. Healthcare providers are being forced to reuse them between patients and sometimes over multiple shifts due to this critical shortage. Social distancing, strict self quarantine, and only seeking medical help when symptoms can no longer be safely managed at home would reduce the viral spread without using critical supplies. N95 masks also need to be properly sized to be effective and the general population would have to be navigating this process on their own. Personal protective equipment is already being tightly rationed nationwide. Just my own 2 cents.
Thank you for this. Please stay safe. I am raising awareness in our community to please donate any masks people may have, especially since some of us in California may have extras from from the forest fires. I absolutely agree, our amazing frontline healthcare providers and staff like you need to be protected first. Stay well. xo Elisa
Please, I need your help with supplies during the qurantine.
Our family is out of cleaning wipes and we can’t find any in the shops.
My granny can’t get out of the home.
I can get N95 masks at http://FreelyTrade.com
Please sell your excess supplies there? We’ll pay WHATEVER the market rate is for it!
You’ll save our lives and our community today!
Stay healthy
Margareta
Hi Margareta – I’m afraid that no one likely has extra supplies right now, and that many are in your situation. I’ll add your comment in case anyone does. Stay well…
First thing I would thank you for sharing such an informative article to make us stay informed about the present crisis. All this work shows that how much time you’ve spent and dedicated to provide such information to help us. Thanks you and loved your blog.
Thank you for sharing the info about the Covid-19 at this time, Symptoms, and precautions for kids.
Thanks for the info about covid-19
you’re so welcome!
Thanks for sharing such beautiful information with us. I hope you will share some more info. Please keep sharing.
What is the company that you use/recommend for covid antibody testing? thank you
I use IGeneX which uses Immunoblot recombinant technology for their IgG and IgM antibodies that is likely more accurate than conventional Western Blot antibody testing, and they also offer a T cell test (IGXSpot) which may be an even better marker for longterm immunity.
Looking forward for better future.
absolutely …